Abscesses in Children
What is an Abscess?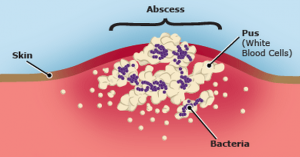
- An abscess is a tender, pus-filled nodule in the skin.
- The affected area is typically red, warm, painful and swollen.
- It may or may not be associated with a fever.
Causes
- An abscess occurs as a result of a bacterial infection of a hair root or skin pore.
- Bacteria that are carried on the skin, typically staph bacteria, may get through a break in the skin barrier and cause an infection.
- A particular type of staph bacteria called methicillin-resistant Staphylococcus aureus, or MRSA, has become a more frequent cause of these infections. The prevalence of this particular type of bacteria in your community may determine which antibiotic your doctor uses to treat the infection.
Typical Course
- When bacteria is introduced underneath the skin, the body combats the infection by walling it off, thereby creating an abscess.
- After about a week, the center of the abscess becomes soft and mushy (filled with pus). The overlying skin then thins out and becomes ready for draining. Without lancing, it will drain by itself in 3 or 4 days. Until it drains, an abscess can be extremely painful.
Treatment
- Antibiotics: Your child’s doctor will likely prescribe an antibiotic that targets the staph bacteria. Treatment with an antibiotic will allow the abscess to heal faster and will reduce the chance of recurrence or further spread to the surrounding skin and tissues.
- Lancing or draining: Contact your child’s healthcare provider instead of trying to drain the abscess yourself, since it needs to be lanced and handled appropriately.
- Simply trying to squeeze the pus out yourself can be very painful. It can also carry the risk that bacteria will be forced into the bloodstream. Squeezing can also result in formation of additional abscesses in the same area
- Once the abscess is opened, it will drain pus for 2 or 3 days prior to healing. Since the pus itself is contagious, the abscess should be covered by a large 4 x 4 inch gauze bandage and tape. Change this bandage and wash the area with an antiseptic soap 2 times a day.
- Supportive measures: Until the abscess comes to a head, apply warm compresses 3 times a day for 20 minutes to help soften the area. Since abscesses can be quite painful, you can also use a pain reliever medication as directed by your child’s physician.
Controlling the Spread of Infection
- Note that pus draining from an abscess is contagious.
- Practice good hand hygiene.
- Make sure that other people in your family do not share your child’s towel or washcloth.
- Promptly wash any clothes, towels, or sheets that are contaminated with pus.
- Used bandages should be carefully thrown away.
Prevention
- Abscesses can be recurrent.
- You can reduce staph bacteria on the skin by washing with an antibacterial soap daily.
- Showers are preferable to baths for decreasing the chances of a recurrent infection.
When to contact your child’s healthcare provider
- The abscess has come to a head and needs to be drained
- The surrounding skin turns red or becomes swollen
- The infection is not better within 48-72 hours after starting the antibiotic.
- You have other concerns or questions.
Download our PDF print version on Abscesses in Children. Please contact our office with any questions.
Allergy
What is an allergy?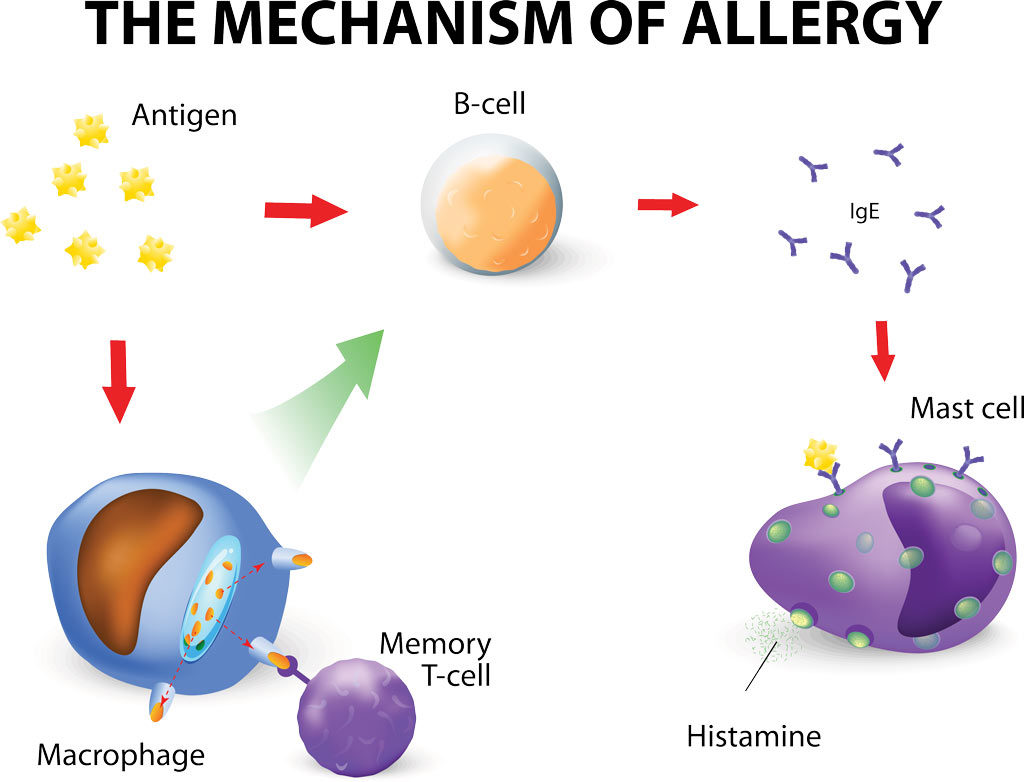
Allergies occur when the immune system that fights off illnesses sees a harmless substance as a threat and reacts to that perceived threat. The substance or allergen can be eaten, breathed in, injected, or simply touched. This allergic reaction can affect different parts of the body causing things such as:
- Anaphylaxis: a severe, life-threatening allergic reaction usually involving swelling, trouble breathing, and can progress to shock
- Asthma: the airways in the lungs swell and constrict. This can be triggered by an allergic reaction but non-allergic triggers are often the cause (viruses, cold air, exercise, smoke exposure, etc)
- Contact dermatitis: a scaly, red, itchy rash caused by touching things like poison ivy, oak or certain chemicals in items like creams, soaps, jewelry, or even nickel in the button of jeans
- Eczema: also called atopic dermatitis; a chronic, itchy, scaly rash not due to a particular substance exposure
- Food allergy: an allergic reaction to food that can range from stomachache to hives to anaphylaxis
- Hay fever: this connotes seasonal allergies, which can cause a runny nose, congestion, watery eyes, and sneezing
- Hives: itchy welts that can by caused by foods, a virus, medicines, or other triggers. Viruses are actually a common cause of hives in young children.
- Insect sting allergy: potentially severe reactions from the sting of yellow jackets, wasps, fire ants, or other stinging insects
- Drug allergy: symptoms such as rashes or more severe reactions from both prescription and over the counter medications
What causes allergies?
Children get allergies from coming into contact with allergens, which can be inhaled, eaten, injected (from stings or medicine), or just touch the skin. Several of the more common allergens are:
- Pollens from trees, grasses, and weeds
- Molds, both indoor and outdoor
- Dust mites that live in bedding, carpeting, and other objects that hold moisture
- Animal dander from animals such as dogs, cats, rabbits, or horses
- Foods and medications
- Stinging insect venom
Read more about allergy testing and treatment at Forest Lane Pediatrics.
Download our PDF print version on Allergy in Children. Please contact our office with any questions.
Asthma
What is asthma?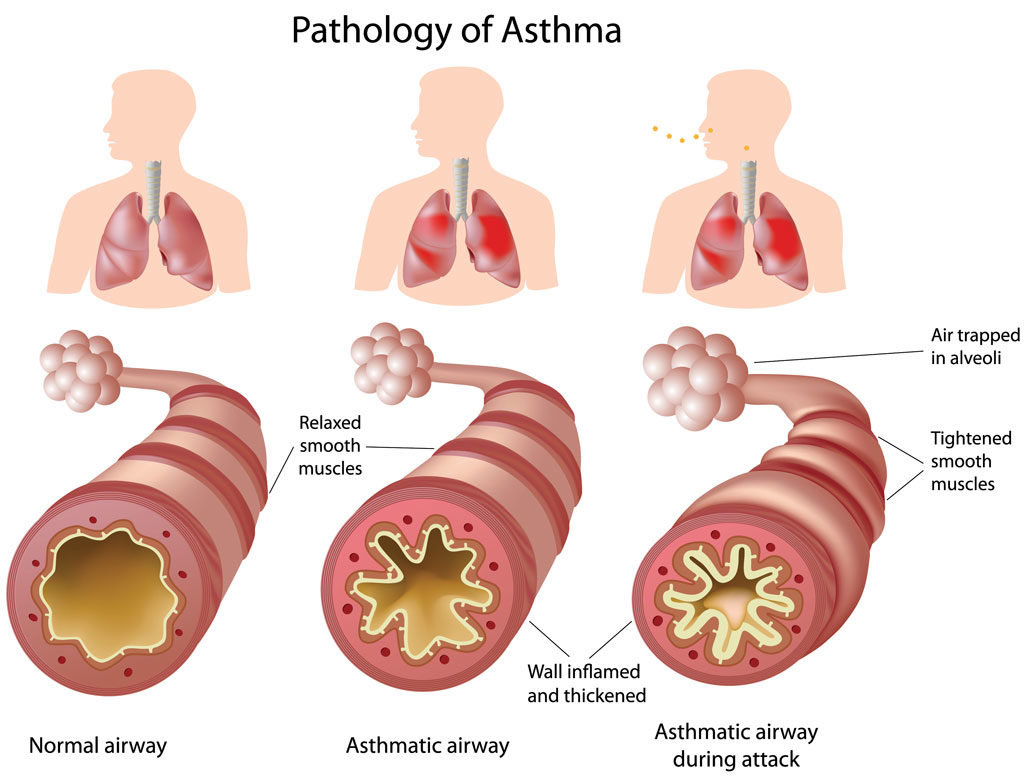
Asthma is a chronic disorder of the airways of the lungs. The airways are reactive and may be inflamed even when symptoms are not present. The extent and severity of airway irritation and consequent symptoms changes over time. The most important goal of asthma management is to control the inflammation in the airways and minimize resultant symptoms.
In an asthma “attack,” the airways can spasm and become narrower. The inner lining of the airways becomes swollen, and the outer muscular lining of the airways constrict, making breathing labored. The good news is that asthma can be treated and controlled.
Who gets asthma?
Asthma is the most common serious chronic illness of children. It is a frequent reason why kids miss school and the most common reason for hospitalization in children. In the U.S., almost 1 out of 10 children has asthma.
Many things can influence when asthma occurs. These include family history (other family members with allergies, asthma, or eczema), infections, exposure to different allergens, tobacco exposure, and exposure to pollution. Children with other types of allergic diseases (food allergy, allergic rhinitis, or eczema) have a higher likelihood of developing asthma.
The prevalence of asthma has been increasing worldwide, but why this is happening is not known.
What are symptoms of asthma?
Some symptoms can appear quickly and others develop over time. Some kids have such frequent or severe symptoms of asthma that they require daily medication. Other children might just need asthma medications intermittently.
A cough may the first and sometimes is the only asthma symptom. Other symptoms can include:
- Wheezing (a high-pitched musical sound)
- Difficulty breathing or feeling short of breath
- Chest tightness
- Reduced exercise tolerance
How is asthma diagnosed?
There is no simple test to diagnose asthma in children. It is often difficult to diagnose in young children. Your child’s physician will ask you specific questions about your child’s history and will then do a thorough physical exam. What you tell the doctor can help determine if your child has asthma. Pertinent questions include:
- Does your child have any symptoms such as wheezing, cough, or feeling short of breath?
- How often do these symptoms occur and how serious are the symptoms? Do they cause your child to miss school or have to sit out from sports? Does coughing keep your child up at night?
- What seems to trigger the symptoms or worsen them? (Common triggers are infections, exercise, smoke, allergens, or stress)
- Is there a history of chronic or frequent runny nose or skin rashes?
- Have any medicines been tried? If so, has anything helped?
- Is there a family history of asthma or allergies?
- If your child sees a lung specialist and is over 5 or 6 years old, he or she may test your child’s lung function with a special machine called a spirometer. The spirometer measures the amount of air the child can exhale and how quickly. It is often helpful to do these measurements before and after medication is used to treat asthma to assess the response.
If your child’s symptoms do not resolve with medications, tests may need to be done to check for other conditions that can make asthma worse or that can masquerade as asthma. Some conditions that can do this are gastroesophageal reflux, vocal cord dysfunction, sinusitis, and even allergic rhinitis.
Asthma can sometimes be tricky to diagnose, and sometimes lung function testing can be normal even in children with asthma. For some children, the tendency to wheeze with colds or other triggers goes away as they grow older.
How is asthma treated?
The goal of asthma therapy is to decrease or completely eradicate symptoms so that children can fully take part in normal physical activities. We can achieve this by avoiding known asthma triggers (such as cigarette smoke) and using asthma medication when needed. It is also a priority to eliminate as much as possible the need for ER visits and hospitalizations due to asthma. If your child is having symptoms of asthma more than twice per week, please make your child’s doctor aware of this. This suggests suboptimal control.
What are triggers of asthma?
Certain things that cause asthma or make it worse are called triggers. It is important to try to discover what those triggers are for your child and to avoid them as much as possible. Allergens and irritants are triggers that are commonly found in home, school, child care, and relatives’ homes. Some frequent triggers are:
- Allergens: Things to which your child might be allergic and which may be a prominent cause of asthma symptoms:
- Dust mites
- Animals with fur or hair
- Cockroaches
- Mice
- Pollens (grasses, weeds, and trees)
- Infections: Viruses such as the common cold or bacterial infection such as pneumonia or sinusitis
- Emotional stress: Crying or laughing hard
Environmental irritants:
- Cigarette or other smoke
- Air pollution
- Cold or dry air
- Sudden weather or temperature changes
- Odors, fragrances, chemicals in sprays
- Unventilated space heaters (kerosene or gas) and fireplaces
- Odors and gases released from new carpets, furniture, or other materials in new homes or buildings
- Exercise: The vast majority of people with asthma can develop wheeze, cough, or shortness of breath when they exercise.
How can your child avoid triggers?
It may be impossible to completely rid your home of all allergens or irritants, but there are reasonable things that you can do to reduce your child’s exposure to triggers. Avoidance of triggers can help you reduce your child’s need for asthma medication.
- Don’t smoke, don’t let your child be exposed to smoke in your home or car
- Dust mite exposure-If your child is allergic to dust mites, then covering your child’s mattress and pillows with dust mite-proof covers and washing bedding weekly can significantly reduce exposure. Vacuuming and dusting often are also recommended.
- Removing carpeting and stuffed animals from the bedroom can also help reduce exposure.
- Reduce exposure to pet allergens: If your child is allergic to certain pets, they should be removed from the home if at all possible. The next best possibility would be to keep the pet out of your child’s bedroom and keep the door closed. A high-efficiency particulate air filter (HEPA) in the bedroom or on the furnace might also help reduce pet allergen levels. Neither of these are as effective as removing the pet from the home.
- Control cockroaches
- Control mice
- Prevent mold: Mold is generally due to excessive moisture indoors, which can result from water damage by flooding, leaky roofs, leaky pipes, or excessive humidity. Repair any source of water leakage. Indoor humidity can be reduced with exhaust fans or a dehumidifier. Existing mold must be cleaned with detergent and water, but if the mold has invaded into the wallboard, some areas may need to be replaced to completely control asthma symptoms from mold.
- Reduce pollen exposure if your child is allergic: Avoiding open windows during high pollen season and using the air conditioner instead can help.
- Reduce indoor irritants: Use unscented cleaning products and avoid mothballs, room deodorizers, and scented candles.
- Check air quality reports: When the air quality is very poor, it is best to keep your asthmatic child indoors as much as possible.
What types of medicines are used?
Asthma can have varied manifestations and differ in each child. Your child’s doctor will decide which asthma medicine is best for your child based on the severity and frequency of symptoms.
Children with only intermittent symptoms can take medicines on an as-needed basis, usually only for short periods. Children with more frequent symptoms may need a daily controller medication. Sometimes more than one medicine is necessary to control and prevent symptoms. If your child has been severely affected, your child’s doctor may
prescribe a few medications at first to quickly gain control and make your child feel better and then try to decrease the medications as your child improves.
Your child’s doctor will probably provide you with an asthma action plan to have at home so that you know exactly what to do on a daily basis and what to do when certain symptoms begin.
Forms of asthma medicine
Asthma medications come in several different forms, including:
- Metered dose inhalers (MDIs)
- Dry powder inhalers (DPIs)
- Liquids used in a machine called a nebulizer
- Pills, chewable, or granule medications
Generally inhaled forms are preferred because they deliver the medicine directly to the lungs with minimal side effects.
Types of asthma medications
Rescue medications: These are medicines that quickly relieve symptoms of wheezing, shortness of breath, and chest tightness. These medicines are usually taken on an as needed basis. With children who have exercise-induced asthma, they can also prevent symptoms if taken before exercise. Albuterol is the most commonly used rescue medication and works by relaxing the smooth muscle of the airways.
Controller medications: These are usually used daily to control asthma and prevent frequent symptoms. They work by decreasing swelling of the airway and some work by causing long-acting relaxation of the airway muscles. Controllers do not help in the acute setting and do not provide any immediate relief. They help over days to weeks to reduce inflammation and usually have maximal efficacy after 2-4 weeks of daily use. Generally, if your child has symptoms more than twice per week during the day or persistent night time cough more than twice per month, a daily controller is indicated.
Controllers medicines include:
- Inhaled steroids-these are the most effective and for that reason the preferred choice. They are very safe and do not cause the serious long term side effects often seen with frequent use of oral steroids.
- Long-acting bronchodilators-these are used in inhalers that also have an inhaled steroid.
- Leukotriene receptor antagonists – they are oral medications that block part of the inflammation cascade and can have benefits against both asthma and allergies.
- Your doctor will talk with you about which agent he or she thinks would work best for your child if one of these is needed.
What devices are used to deliver asthma medicines?
Medicines for asthma can be given to your child using different devices. These include:
- Nebulizer: This uses an air compressor and cup to vaporize the liquid medication into a mist your child can breathe in. In order for optimal delivery of the medicine to the lungs, these medications must be given with a mask (for babies and small children) or a mouthpiece (for older children to adults).
- Metered dose inhaler: This is the most frequently used device for asthma medications. Spacers or aero chambers, which attach to the inhaler significantly improve the delivery of the medication to the lung and decrease oral absorption. This enhances the efficacy and decreases side effects. There is one new controller inhaler on the market now that has its own chamber, Aerospan, which is licensed for children 6 and up.
- Dry powder inhaler: This device is available for some medicines. It does not require coordination of breathing in with pressing a button, but it does require training and is not generally used in children less than 4.
- Peak flow meter: A peak flow meter can be used with children over 6 to have a baseline level of how fast air can be blown out. Your child’s doctor may recommend one for asthma monitoring.
Asthma and School
Since children spend most of their waking hours at school, it is very important that asthma symptoms can be managed there. It is a good idea to let the school know that your child has asthma and have medications for use if your child develops any persistent cough or shortness of breath.
Communication with the school is vital to proper asthma management for your child.
- Think about meeting with your child’s teachers, the school nurse, and coaches at the beginning of the school year to let them know about your child’s asthma, how serious it is, and what medicines your child takes, as well as what to do in the event of an emergency.
- Ask your child’s doctor to fill out an asthma action plan for the school as well as a permission form that includes whether your child can be allowed to carry and use his own inhaler and spacer.
- Sign a release at school and your child’s doctor’s office to allow an exchange of medical information between you, the school, and your child’s doctor.
- Ask the school nurse about its policies on how your child will have access to his medicines and how they deal with emergencies during field trips and after school activities.
- Ask for updates as necessary. The school should also let you know about changes or problems with your child’s symptoms while he is at school.
Help your child manage his asthma at school.
- Talk with your child about how well is his asthma is being handled at school. Also talk with your child’s teachers, school nurse, coaches, or other school personnel about how well your child is coping with asthma at school.
- Students with asthma face additional hurdles at school, which can include:
- Missing school because of asthma symptoms or doctor visits
- Avoiding school or school activities. If your child’s asthma is under suboptimal control, he might avoid exercise, as that can be a trigger. Exercise is one trigger we do not want your child to avoid long term, but sometimes better medication management is needed to allow your child to consistently exercise without triggering asthma symptoms.
- Your child might be struggling because he is not taking his medicine before exercise as instructed. She might not want to go to the nurse or office to use her inhaler before exercise, but then she might feel bad and avoid exercise if she does not use it. If your child is old enough and responsible for using his inhaler properly independently, most schools will authorize her to carry the inhaler with her to avoid this problem.
Summary
Asthma is a chronic disease of inflammation and constriction of the airways. Depending on the frequency and severity of your child’s symptoms, your child’s doctor will prescribe medications to minimize symptoms and maximize your child’s ability to participate fully in life. Besides medication, avoiding those triggers that are avoidable (such as cigarette smoke) can help reduce the need for medication. Your child’s doctor might also recommend allergy testing to see if allergy plays a significant role in your child’s asthma.
While there is no one perfect medicine that controls all asthma, most children’s asthma can be well controlled to minimize symptoms and maximize your child’s ability to take part in things he enjoys. We also want to make sure your child’s symptoms are well controlled at school and that he has any needed rescue medications at school.
If you have questions about your child’s asthma, please call your child’s doctor or set up an appointment so that he or she can examine your child and answer your questions fully for you.
Download our PDF print version on Asthma in Children. Please contact our office with any questions.
Bloody Nose (Epistaxis)
Nosebleed Basics
The nose has a rich blood supply and nosebleeds (or epistaxis) are very common in children. They are often caused by dryness of the nasal lining, coupled with the normal rubbing and picking that all children do when their noses are blocked or itchy. Vigorous nose blowing or nasal suctioning can also cause bleeding. Children who have nasal allergies are more likely to have nosebleeds because they rub and blow their noses more often. Antihistamines can also dry the nose and result in bleeding. In addition, being hit in the nose or other injuries may cause nosebleeds. Fortunately, you should be able to stop the bleeding if you use the correct technique.
Managing Nosebleeds
Over 99% of nosebleeds will stop following 10 minutes of direct pressure if you press on the right spot.
- Have your child sit up, lean forward (not backward), and spit out any blood. Swallowed blood is irritating to the stomach. Don’t be surprised if your child vomits a small amount of blood or passes a dark stool the following day.
- Gently pinch the soft part of the lower nose between your thumb and forefinger for 10 minutes. If your child is old enough, teach him how and where to hold his own nose. Have your child breathe through his mouth. Don’t release the pressure for a full 10 minutes. If the bleeding continues, you may not be pressing on the right spot. Readjust your pressure point and try again.
- If the bleeding persists, insert a gauze covered with petroleum jelly (Vaseline or Aquaphor) or water-based jelly (K-Y) into the nostril. Squeeze again for 10 minutes. Leave the gauze in for another 10 minutes before you remove it. If bleeding still continues, call your child’s healthcare provider while continuing to hold pressure in the meantime.
Common Mistakes
- A cold washcloth applied to the face will not help stop nosebleeds.
- Pressing on the bony part (bridge) of the nose will not be effective in controlling the bleeding.
Prevention
- Help the area heal by applying a small amount of petroleum jelly twice a day to the center wall inside the nose (the septum) with a cotton swab.
- Use a humidifier to reduce the dryness of the air in your home.
- Loosen up dried mucus. Get your child into the habit of putting 2 or 3 drops of warm water or nasal saline drops in each nostril prior to blowing a stuffy nose.
- Avoid certain medications. Aspirin can increase the tendency of the body to bleed easily for up to a week and can make nosebleeds last much longer.
- Treat your child’s nasal allergies. Talk to your doctor about optimizing treatment for allergic symptoms to break the itching-bleeding cycle and to minimize trauma to the nasal lining.
- Avoid exposure to nasal irritants, especially cigarette smoke.
Seeking Medical Care
- Call immediately if the bleeding does not stop after 30 minutes of direct pressure.
- Call during office hours if nosebleeds are a frequent problem or if you have additional concerns or questions.
Download our PDF print version on Bloody Nose Epistaxis in Children. Please contact our office with any questions.
Bronchiolitis
What is bronchiolitis?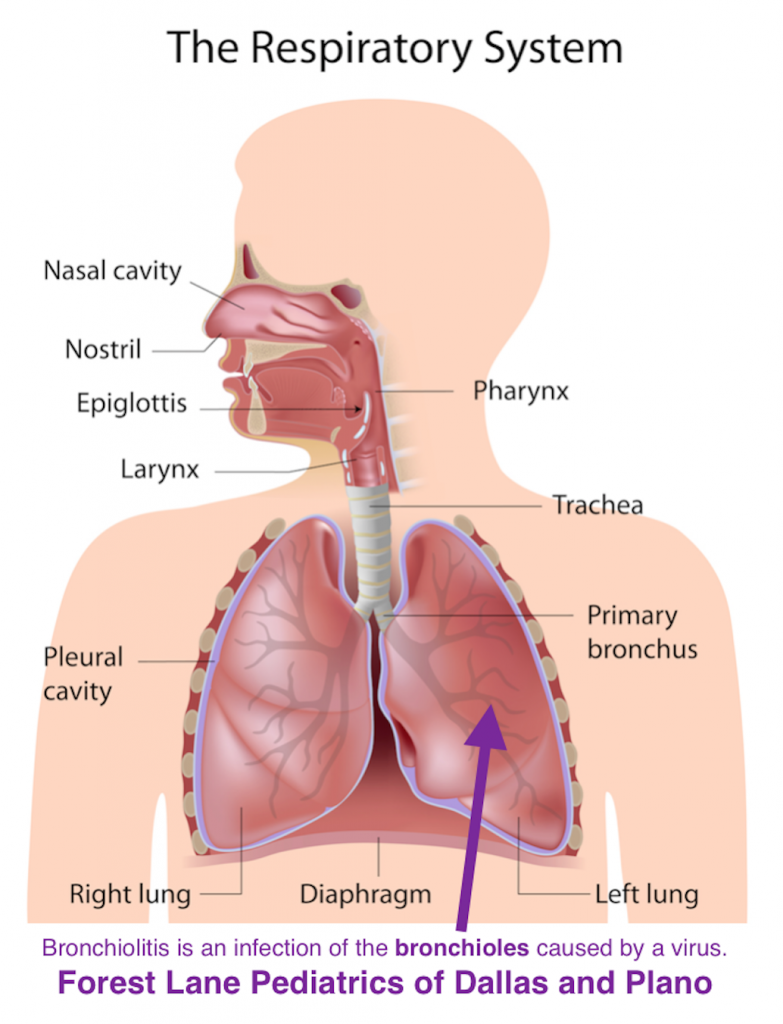
Bronchiolitis in Children (PDF)
Bronchiolitis is a medical term for a viral chest infection.
What is the cause?
Bronchiolitis can be caused by several different viruses. The best-known virus is Respiratory Syncytial Virus (RSV). The virus attacks the small airways of the lungs (bronchioles). As a result, these airways become swollen and fill with mucus. This leads to breathing difficulty in some babies and children.
When does it occur?
Bronchiolitis can occur year round but is most often seen in the winter.
Who is at risk?
Infants and small children are most likely to contract the illness. The illness can be more severe in young infants under 6 months old, especially premature infants or infants with medical disabilities.
What are the symptoms?
The illness can have various presentations but most often starts off as a common cold then followed by a “wet” cough and sometimes breathing difficulty. Some babies may begin to “wheeze” which sounds like a high-pitched whistling sound. Babies often will develop a fever with their illness in the first few days. Serious symptoms that require immediate medical attention include rapid or difficult breathing, lethargy, or poor liquid intake.
How long does it last?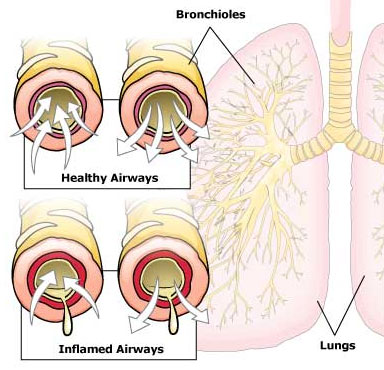
Wheezing and trouble breathing usually develops within the first few days of illness and may last anywhere from a few days to 2 weeks. Children are thought to be most contagious the first week of the illness.
What are some complications?
- Breathing difficulty is the number one issue with bronchiolitis. Most babies are successfully treated at home but some may need to be hospitalized to help monitor breathing and provide oxygen.
- Dehydration: Due to thick mucus that develops in the nose and lungs, many babies have de-creased intake of liquids during the illness. Most babies can be coaxed to drink enough fluids at home, but some babies will require IV hydration in the hospital or emergency room.
- Ear infections and pneumonia are not uncommon with children with bronchiolitis. Though most babies will not need antibiotics, it is best to have your child examined at the onset of illness and if symptoms worsen in order to diagnose these conditions early.
- Asthma is by definition an airway disease caused by recurrent wheezing. About 30% of babies with bronchiolitis will go on to have some form of Asthma.
How can I take care of my child?
- Hydration: This is probably the most important thing you can do to help your child. We recommend continuing to nurse or formula feed your baby as much as possible. If they are not interested in either, we encourage families to offer Pedialyte instead. If your baby is taking less than half their normal volume or having less than 3 wet diapers a day, you should seek out medical attention quickly.
- Nasal suctioning is highly recommended. All babies need to breathe through their nose often. If their nose becomes blocked, nursing or bottle-feeding will become difficult. Suction alone can-not remove dry secretions. We recommend saline nasal drops to loosening up mucus. Place three drops of saline in each nostril. After about one minute, use a soft rubber suction bulb to suck out the mucus. You can repeat this procedure several times until your child’s breathing through the nose becomes quiet and easy.
- Albuterol: You may have been prescribed albuterol through a nebulizer or inhaler to help treat the cough and wheezing. Albuterol is often used for asthmatics to control their breathing. Though Albuterol works for some children with bronchiolitis, it may not be helpful for your child. Please discuss medication options with your provider treatments for cough or wheezing. Your provider should give a schedule of treatments if albuterol or other prescriptions are given.
- Fever reducers: You can give your baby acetaminophen every 4 to 6 hours as needed for fever over 101 degrees F. You may also use ibuprofen every 6 to 8 hours for babies over 6 months.
- Cold medications: In general, cold medications will not help with bronchiolitis. Please discuss further with your provider.
- Humidity: Warm or cool humidifier may help to keep the air around the baby moist and help them to breath easier.
- Smoking: Please don’t smoke around the baby. Smoke has been shown to increase the severity of bronchiolitis.
When should I call the office?
Call IMMEDIATELY if:
- Fast (60 breaths or more per minute) or labored breathing.
- Baby is wheezing constantly.
- Any fever over 100.4 degrees F in infants under 2 months old.
- Unable to take down any liquids for more than 12 hours.
Call during business hours if:
- For babies over 2 months, any fever lasting more than 3 days. Fever is defined as temperature over 101 F for this age group.
- The cough is not improving within 2 weeks.
- You have other questions or concerns.
Colic in Babies
Colic Basics
- Colic refers to bouts of unexplained crying and fussiness (not due to pain or hunger).
- It can affect up to one-fifth of babies.
- Crying episodes can last for 2-3 hours at a time and often intensify in the early evening.
- During crying spells, babies may scream, extend or pull up their legs, and flex their arms. Sometimes, their abdomens may appear tense from crying or distended from swallowing a lot of air.
- Colic usually starts by the 2nd or 3rd week of life and usually peaks by 6 weeks of
- age, when the episodes tend to last 3 hours at a time. Gradually, the duration of the crying declines and usually resolves by 3-4 months of age (although it may persist up to 6 months of age).
Causes
Although there has been extensive scientific research on colic, no one knows exactly what causes it. Colic tends to occur in babies that are more sensitive to their surroundings. Hyperstimulation can overwhelm the immature nervous system’s ability to “self-soothe.” As the baby matures, this inability to self-console (marked by excessive crying) will improve.
Colic is not the result of bad parenting, so don’t blame yourself. Remember that babies are “born with” colic. Unfortunately, there is no “magic pill” to eliminate colic. The best treatment is time, and all babies will eventually outgrow it. Consult with your pediatrician if it seems like your baby is chronically “colicky” and not just fussy for specific periods during the day. Your doctor can discuss any additional symptoms and help determine whether your child has a medical diagnosis like GERD (acid reflux/heartburn) or cow’s milk protein allergy.
Comfort Techniques
Fussy crying related to colic will not cause any harm to your baby. Although the crying can’t be completely eliminated, you may be able to comfort your baby and reduce the crying with the following methods:
Rhythmic motions. A soothing, rhythmic activity is one of the best ways to help a baby relax. The following techniques may allow you to help your baby settle down and fall asleep:
- cuddling your child in a rocking chair
- rocking your child in a cradle or bassinet
- swaying side to side while holding your child
- placing your child in a windup swing or vibrating chair
- holding your baby while bouncing on an exercise ball
- going for a stroller ride (outdoors or indoors)
Swaddling or snuggling. This will help your baby feel secure and warm. Swaddling (using a thin blanket) is especially helpful for calming younger babies and can help increase sleep duration. Alternatively, you can place your child in a baby sling or wrap, which keeps her close to you while freeing up your hands.
Calming sounds. This can minimize outside stimuli and help soothe the baby by mimicking the environment of the womb. Try a white noise machine, or run a fan, vacuum, or washer/dryer.
Using a pacifier. The act of sucking is comforting for babies, and a pacifier may be able to provide instant relief.
Feeding strategies
- If you’re nursing, you can try to eliminate milk products, caffeine, onions, cabbage, and any other potentially irritating foods from your own diet.
- If you’re formula feeding, consider a protein hydrolysate formula. If food sensitivity is causing the discomfort, the crying symptoms should decrease within a few days of these changes.
- Avoid over-feeding your baby, which could make her even more uncomfortable.
Survival Tips
- Get rest when possible and ask for help. Avoid fatigue and extreme exhaustion. Try to nap at least once a day, in case the night goes badly. Ask your partner, friend, neighbor or relative for help around the house and with baby care so that you can get a break.
- Caring for a colicky baby is a two-person job.
- Take breaks. Make sure you have opportunities to get out of the house and clear your mind. These breaks are not acts of selfishness—instead, they will allow you to better nurture and care for your baby.
- Talk to someone regularly about your mixed feelings. All parents have contradictory feelings towards their babies. You can still love your child even amidst frustration by her colicky episodes. If you are having difficulty coping, be sure to discuss this with your doctor.
- Beware of gimmicks. Many colic ‘treatments” make extraordinary but unregulated claims. The medicines on the market for colic are often ineffective and some may even be dangerous for children of this age. Talk to your child’s doctor about his or her recommendations regarding these treatment options.
Seeking Medical Attention
Call IMMEDIATELY if:
- Your baby cries inconsolably for more than 3 hours.
- You are afraid you might hurt your baby.
- Your baby is acting very sick.
Call during office hours if:
- You are having difficulty finding ways to soothe your baby’s crying.
- The crying continues after your baby reaches 4 months of age.
- You think your baby may be hungry and not gaining weight.
- You have other concerns or questions.
Download our PDF print version of Colic. Please contact our office with any questions.
Common Colds
Common colds are extremely “common!” Children may catch as many as 8-10 viral infections per year in the first few years of life. Cough, congestion, runny nose, sneezing, and mild fever are typical symptoms of a cold. The common cold is caused by a virus, and it may take 7-10 days to run its course. Coughs may linger for a week or more past that. Viral infections do not respond to antibiotics, but there are several things you can do to help your child feel better during an illness.
Symptomatic care: During a common cold, a child’s mood, appetite, and sleep may be affected. The goal is to provide temporary symptom relief while allowing the child’s body to fight the infection.
- Nasal saline Saline irrigation of the nasal passages can help flush out drainage and mucous. For younger babies, suctioning with a “blue bulb” or a NoseFrida device can help. Older kids and adults may benefit from using a Neti Pot or NeilMed Sinus Rinse.
- Humidifier A cool-mist humidifier can loosen congestion and help a child breathe more comfortably at night. Be sure to clean out the humidifier according to manufacturer’s instructions.
- Vicks BabyRub This is a mild and safe product that has been shown to decrease a nighttime cough. It is safe for babies 3 months and older. VapoRub is safe for age 2 years and older.
- Fever Control Fever is a sign that the body is fighting an illness appropriately. High fever makes a child feel uncomfortable, but it is not harmful to the body. Infants less than 2 months of age with a rectal temperature of 100.4 or higher require immediate evaluation in a pediatric emergency room, but for older kids, fever is not usually an urgent matter. Acetaminophen can be given for a child’s comfort, and for kids 6 months and older, ibuprofen is preferred for pain and fever control. Dosing depends on your child’s weight.
- Honey Honey should not be given to children less than 12 months of age, but for older kids, honey or honey-based cough syrups can be given to help with cough.
- Cough and Cold Medications Unless your doctor specifically prescribes a medication, the above measures will be safer and more effective than medicines for your child’s symptom relief. The American Academy of Pediatrics strongly recommends that over-the-counter cough and cold medications not be given to kids younger than 2 years because of the risk of life-threatening side effects. Also, several studies show that cold and cough products don’t work in children younger than 4 years and can have potentially serious side effects.
- Antibiotics As previously mentioned, antibiotics are not necessary for common colds. However, common colds will sometimes lead to secondary bacterial infections such as ear infections, sinus infections, bronchitis, or pneumonia. These are very unlikely to be present in the first few days of an illness. If fever, fussiness, sleep disturbance, and cough seem to be worsening by the 4th or 5th day of a common cold, a secondary infection may be developing. An examination in the office is necessary to make this diagnosis and prescribe appropriate treatment.
Common Cold Advice
Viral Upper Respiratory Infection (URI):
The common cold is caused by viruses. Over 100 serotypes of rhinoviruses are responsible for approximately 50% of all colds. The other 50% are caused by parainfluenza, RSV, coronavirus, and enteroviruses. Colds are not caused by bacteria or exposure to cold air. Viruses cannot be killed with antibiotics. Viruses cause illness by taking over some of the cells in the body in order to multiply. In the nose, this leads to injury of the cells causing a runny nose and congestion. Fever is a direct result of the immune system fighting the virus.
Typical symptom pattern
- Fever up to 3 days.
- Sore throat up to 5 days (with other cold symptoms)
- Nasal discharge and congestion up to 14 days.
- Cough up to 21 days.
- Patients may also have sneezing, irritability, poor sleep and poor appetite.
If your child is not following the typical symptom pattern, you should bring her in to be examined or re-examined by one of our doctors.
Typical Timing:
- 6 to 8 colds per year for children 6 years old and younger.
- 8 to 12 colds per year for children who attend daycare.
- Symptoms last an average of 14-21 days.
- The highest frequency of colds occurs in the Fall and Winter.
- 80% of patients with symptoms lasting more than 2 weeks still have an uncomplicated viral URI.
Treatment Options
5 things can be done safely:
- Nasal suction with any nasal saline drops. Most parents find that the NoseFrida is more effective than the typical bulb suction and can be used to remove mucus from your child’s nose. It is available at some local stores or online at www.amazon.com or other retailers. This can be done as frequently as needed (safely). However, if your child’s nose begins to bleed, you may want to take a break from this and apply some Vaseline 3 to 4 times day to any raw areas.
- Putting a humidifier in a child’s room at night can help their cough.
- Elevating the head of the bed may help with mucous drainage. Be careful that the baby does not roll down!
- For children over 1 year of age, 1-2 teaspoons of honey (mixed with water/lemon or given by itself) can be given every 6 to 8 hours as needed, which may help reduce coughing.
What about Cold and Cough Medicines?
Forest Lane Pediatrics and the American Academy of Pediatrics DO NOT recommend cold and cough medicines for children.
- Not proven to help.
- May cause dangerous side effects.
There is little to no evidence that cold/cough medicines work in children. Since October 2008, no FDA-approved OTC cold and cough medicines are available in the U.S. for children 4 years old or younger.
Contagiousness & Prevention
- Viral URI’s are most contagious during the first 2 to 4 days of symptoms.
- Cold viruses can be detected on children’s hands for 2 hours.
- Some cold viruses can live on surfaces for 24 hours.
- Cold viruses are transmitted through respiratory droplets or touch.
- Emphasize hand washing with soap and warm water. (www.cdc.gov/handwashing).
- Anti-virus phenol/alcohol cleaning products (Lysol©) may help reduce transmission.
- The development of an effective vaccine for the common cold is unlikely because of the diversity of viruses and virus subtypes responsible.
Symptoms of Secondary Bacterial Infections
5-10% of children with viral URI’s develop secondary bacterial infections. The most common are ear infections, sinus infections, and pneumonia. Suspect a bacterial infection and contact our office if you notice any of the following:
- Fast, labored or difficult breathing.
- Fever for more than 3 days.
- Fever that goes away for 24 hours or longer, but then returns.
- Ear pain or discharge.
- Sore throat for more than 5 days.
- Nasal discharge for more than 14 days.
- Cough for more than 21 days.
Viral URI Symptom Details
Nasal congestion and nasal discharge usually signal the beginning of a viral URI.
The mucus is usually clear for the first few days, cloudy for several more, and then clear at the end of the cold. Mucus that has been in the nose or throat for longer than one day is usually a cloudy yellow or green color. Enzymes that are a part of your immune system cause the mucus to change color. Non-clear mucus is not a sign by itself of a bacterial infection or that antibiotics are needed. Congestion is usually the worst on days two to six of the illness.
Cough usually begins shortly after the nasal congestion starts.
Most coughs represent the body’s effort to protect the airway.
When mucus slides down the windpipe from the nose, it stimulates a cough reflex in order to keep the mucus from going into the lungs.
Babies are not efficient coughers, so they tend to have more difficulty clearing their airway, especially when they are lying down. For this reason, sleeping with the head above the chest can improve coughing in babies. Come into the office for a severe cough, especially with fast or labored breathing.
Sore throats are usually caused by viruses.
Sore throats caused by viruses usually start to improve after several days and are usually gone by day six or seven of illness. Blisters in the mouth or throat are usually caused by viruses.
Group A streptococcus is the bacteria that causes “strep throat” and can usually be distinguished from a viral URI sore throat because strep throat patients usually don’t have other viral URI symptoms except fever.
Fever can mark the beginning days of a viral URI.
Usually, fever caused by a virus resolves after two to three days, but it can last up to one week. Older children can be observed for a day or two if there is no obvious other source of fever (i.e. burning with urination, ear pain, or trouble breathing).
Infants less than three months of age (90 days old) with a temperature of 100.4 or more rectally, should be discussed with a doctor immediately. If fever persists in any child for longer than 2-3 days, lasts for longer than 2-3 days after a visit in our office, or returns later in the illness, the child should be re-examined and/or discussed over the telephone to be certain that a secondary bacterial infection is the cause of the current fever.
Return to school or daycare
Your child can return after the fever is gone for 24 hours and your child feels well enough to participate in normal activities. The spread of colds cannot be completely prevented.
Download our PDF print version on Common Cold Advice. Please contact our office with any questions.
Concussion Treatment
Concussion Return to Learn/Play Protocol
Like any injury, rest is a key component of healing. Unfortunately, a child’s brain recovers more slowly than adults and on average it will take a middle school student 4+ weeks and a high school student 2-3 weeks to fully recover. To help your child’s brain recover as quickly as possible, follow the protocol below. Each stage of the protocol should take a minimum of 24 hours to complete. If symptoms worsen on one stage of the protocol, the child should immediately rest until all symptoms have resolved and then resume the protocol at the stage prior to the one in which symptoms developed.
Return to Learn
Stage 1: Home – Total Rest
Activity: Complete cognitive rest
- No mental exertion – no computer, texting, video games or homework.
- Stay at home
- No driving
Objective: Recovery
Stage 2: Home – Light Mental Activity
Activity: Slowly reintroduce cognitive activities
- 5-15 minutes mental exertion
- No prolonged concentration
- Stay at home
- No driving
Objective: Gradual controlled increase in cognitive activities
Stage 3: Home – Increased Mental Activity
- Homework in longer increments
- Initially 20-30 minutes
- Provide quiet place for scheduled mental rest
Objective: Increase cognitive stamina by repetition of short periods of cognitive activity
Progress to the next level when able to handle 30-40 minutes of mental exertion without worsening of symptoms and able to tolerate 1-2 cumulative hours of homework at home.
Stage 4: School – Part Time
- Half day of school with accommodations
- No standardized testing
- Modified classroom testing
- Provide extra time, extra help, and modification of assignments
Objective: Re-entry into school with accommodations to allow for increased cognitive load
Stage 5: School – Full Time
- Full time school with minimal accommodations
- No standardized testing, routine tests ok
- Continue decrease of extra time, help, and modification of assignments
- May require more supports in academically challenging subjects
Objective: Accommodations decrease as cognitive stamina improves
Progress to the next level when able to handle 60 minutes of mental exertion without worsening of symptoms.
If student is an athlete, he/she may begin the Return to Play Protocol at step 2.
Stage 6: School – Full Time
- Attends all classes
- Full homework
- No accommodations
- If symptoms continue beyond 3-4 weeks, prolonged in-school support is required and the parent should request a 504 plan meeting.
Return to Play
Stage 1: No Activity
- Complete cognitive (e.g. mental) rest
Objective: Recovery
Stage 2: Light aerobic exercise
- Walking, swimming or stationary bicycle keeping intensity less than 70% of maximum predicted heart rate
Objective: Increase heart rate
Stage 3: Sport- specific exercise
- Skating drills in ice hockey, running drills in soccer
- No head impact activities
Objective: Add movement
Stage 4: Noncontact training drills
- Progression to more complex training drills, e.g. passing drills in football and ice hockey
Objective: Exercise, coordination and use of brain
Stage 5: Full contact practice
- Following medical clearance, participate in normal training activities
Objective: Restore confidence and allow coaching staff to assess functional skills
Stage 6: Return to play
What is a concussion?
A concussion is a disturbance in brain function caused by a direct or indirect force to the head. It results in a variety of nonspecific symptoms (like those listed below) and often does not involve loss of consciousness. Concussion should be suspected in the presence of any one or more of the following:
- Symptoms (such as headache), or
- Physical signs (such as unsteadiness), or
- Impaired brain function (e.g. confusion) or
- Abnormal behavior.
Concussion Symptoms
The following are symptoms of concussion. When the answers to these questions reflect the baseline score (score the student would have achieved prior to the concussion – should be zero), then the student can progress to the next level of the return to play guidelines above. For each question the student should choose the score that reflects how he is feeling at that time. A score of 0 reflects absence of the symptoms while a score of 6 indicates the symptoms are severe. The total of the points accumulated can help the student and parent monitor for resolution of symptoms.
How do you feel?
Headache
0 1 2 3 4 5 6
“Pressure in head”
0 1 2 3 4 5 6
Neck Pain
0 1 2 3 4 5 6
Nausea or vomiting
0 1 2 3 4 5 6
Dizziness
0 1 2 3 4 5 6
Blurred vision
0 1 2 3 4 5 6
Balance problems
0 1 2 3 4 5 6
Sensitivity to light
0 1 2 3 4 5 6
Sensitivity to noise
0 1 2 3 4 5 6
Feeling slowed down
0 1 2 3 4 5 6
Feeling like “in a fog“
0 1 2 3 4 5 6
“Don’t feel right”
0 1 2 3 4 5 6
Difficulty concentrating
0 1 2 3 4 5 6
Difficulty remembering
0 1 2 3 4 5 6
Fatigue or low energy
0 1 2 3 4 5 6
Confusion
0 1 2 3 4 5 6
Drowsiness
0 1 2 3 4 5 6
Trouble falling asleep
0 1 2 3 4 5 6
More emotional
0 1 2 3 4 5 6
Irritability
0 1 2 3 4 5 6
Sadness
0 1 2 3 4 5 6
Nervous or Anxious 0 1 2 3 4 5 6
Total Concussion Symptom Score: ________________
Download our PDF print version on Concussion Treatment for Children. Please contact our office with any questions.
Constipation (Encopresis)
Most children who are significantly constipated become so over a long period of time, and it generally takes a fairly long period of time to completely manage the constipation, so it is wise to expect your child will need to be on treatment for at least 2 months. It is not uncommon to need treatment for over 6 months.
When children develop constipation, their stools are hard, and the walls of the colon dilate significantly. This dilation of the colon can occur at the rectum as well, which stretches the nerve endings and sometimes decreases sensation. This can have the effect of soft stool leaking around the hard stool without any sensation on your child’s part, leading to staining and accidents.
While it might seem strange that a child who is having messy accidents has constipation and not diarrhea, most children with soiling simply have it due to the reasons above, and it cannot be effectively managed without medical treatment to soften the stools. It is important to realize that your child is not having accidents on purpose, and at this point, truly has no control over it. It is our job to manage your child’s constipation, thereby softening the stools, which over time allows the colon size to return to normal and allows full sensation to return. It may take a few weeks or longer for soiling accidents to completely stop, but if your child is having daily soft stools, he or she is on the right track towards resolving the soiling problem. Our goal is for your child’s stool to be so soft that it is completely painless to have a bowel movement. We also want your child to have a bowel movement at least every other day. Once the stool is consistently coming out soft, that is a sign your child is on the right dose of daily medicine. If the stools are loose and watery, the amount of medication might be too much, and we can back down a bit. Conversely, if your child has been on the medicine for a few days and is still having hard stools, additional medication might be needed. Please call the office if stools are still hard or painful or if they are watery.
We recommend that your child stays on treatment at least 2 months after the stools are soft and painless. After this time, we can try to gradually wean the medicine off.
- Once your child is doing well on the medicine, one way to make sure he or she stays regular is to make sure they get plenty of fluid as well as fiber.
- Daily servings of fruits and vegetables (target is 5-9 servings a day) will help ensure your child gets enough fiber. High-fiber cereals (look for at least 5-7g fiber per serving) can help as well. Some good brands are Post Raisin Bran, Fiber
- One Honey Oat Clusters. Oatmeal also has fairly high fiber content, particularly if your child has more than 1 serving at a time.
- Remember to encourage your child to drink plenty of water and a little bit of juice each day to make sure stools stay soft.
Medication
Miralax 1 capfull in 8 ounces of clear liquid 2-3 times a day for 2 weeks or until there are no more chunks in the stool, then give decrease as needed for 1-2 soft stools per day for a minimum of 2 months.
Download our PDF print version of Constipation in Children. Please contact our office at with any questions.
Diarrhea
What is diarrhea?
Diarrhea is defined as the sudden increase in the frequency and looseness of bowel movements (BMs). Mild diarrhea is the passage of a few loose or mushy BMs. Severe diarrhea is the passage of many watery BMs. The best indicator of the severity of the diarrhea is its frequency. The main complication of diarrhea could be dehydration from the loss of too much body fluid.
Symptoms of dehydration are a dry mouth, the absence of tears, infrequent urination (for example, none in 12 hours, or less than 3 urine voids in 24 hours), and a darker, concentrated urine. The main goal of diarrhea treatment is to prevent dehydration.
What is the cause?
Diarrhea is usually caused by a viral infection of the lining of the intestines (gastroenteritis). Sometimes it may be caused by bacteria or parasites. Bacterial causes of diarrhea are more likely to result in blood in the stool or crampy abdominal pain.
How long will it last?
Diarrhea from a viral infection usually lasts several days to 2 weeks, regardless of any type of treatment. The main goal of treatment is to prevent dehydration. Your child needs to drink enough fluids to replace the fluids lost in the diarrhea. Don’t expect a quick return to solid bowel movements.
What should I feed my child?
For frequent, watery diarrhea:
- Fluids: Encourage your child to drink plenty of fluids to prevent dehydration. Give your child water or Pedialyte as the main fluid for the first 24 hours of watery diarrhea. A child who is taking table foods doesn’t need to get calories from milk. On day 2, offer some milk as well as water. Avoid fruit juices and sweeter fruits, because they all make diarrhea worse. Bananas, apples, and applesauce are ok. If your child refuses solids, give your child milk (or formula) rather than water. Diarrhea can cause a temporary lactose intolerance, so you may need to switch to soy milk, lactose-free milk, or Pediasure temporarily.
- Table foods: Keep giving your child table foods while he has diarrhea. The choice of food is important. Starchy foods are digested best. Examples of such foods are dried cereals, grains, bread, crackers, rice, noodles, and mashed potatoes. Pretzels or saltine crackers can help meet your child’s need for sodium. On the second day of the diarrhea, soft-boiled eggs, bland meats, and yogurt are easily digested and provide some protein.
For mild diarrhea (loose BMs):
- Follow a regular diet with a few simple changes:
- Eat more foods containing starch. Starchy foods are easily digested during diarrhea.
- Examples are cereal, breads, crackers, rice, mashed potatoes, and noodles.
- Drink more water. Avoid all fruit juices and carbonated drinks.
- Milk and milk products are fine.
- Avoid beans or any other foods that cause loose bowel movements.
How can I take care of my child?
- Avoid over the counter anti-diarrhea medications as they can be dangerous in children.
- Probiotics contain healthy bacteria (lactobacilli) that can replace unhealthy bacteria in the GI tract. Yogurt like DanActive or Activia are a good source of these bacteria. If your child is over 1 year old, give 2 to 6 ounces (60 to 180 ml) of yogurt twice daily. Another option is a probiotic supplement like Culturelle Kids, Florastor Kids, FloraQ, or VSL#3. These powders have live bacteria that can be added to any food or drink 1-2 times daily and are found at many pharmacies or health food stores.
- A multi-vitamin containing zinc and iron may help the intestines to heal and may slow down the diarrhea.
- Diarrhea can be very contagious. Always wash your hands after changing diapers or using the toilet. This is crucial for keeping everyone in the family from getting diarrhea.
- The skin in the diaper area can become irritated by the diarrhea. Wash the area near the
- anus after each bowel movement and then protect it with a thick layer of petroleum jelly or other diaper ointments. This protection is especially needed during the night and during naps. Changing the diaper quickly after bowel movements also helps.
- For children in diapers, diarrhea can be a mess. Place a cotton washcloth inside the diaper to trap some of the more watery BM. Use disposable superabsorbent diapers to cut down on cleanup time. Use the diapers with snug leg bands or cover the diapers with a pair of plastic pants. Wash your child under running water in the bathtub.
- If your child has vomited more than twice, follow your doctor’s recommended treatment for vomiting instead of this treatment for diarrhea until your child has gone 8 hours without vomiting.
When should I call my child’s healthcare provider?
Call IMMEDIATELY if:
- There are signs of dehydration (no urine in more than 12 hours, very dry mouth, no tears).
- Any blood appears in the diarrhea.
- The diarrhea is severe (more than 8 BMs in the last 8 hours).
- The diarrhea is watery AND your child also vomits repeatedly.
- Your child starts acting very sick.
Call during office hours if:
- Mucus or pus appears in the BMs.
- A fever lasts more than 3 days.
- Mild diarrhea lasts more than 2 weeks.
- You have other concerns or questions.
Diarrhea Diet
(4 months to 1 year old)
- No Juice
- Continue regular formula
- Pedialyte
- May give potatoes (baked, boiled, or mashed)
- Pasta
- Rice Products
- Cereal
- Probiotics (pharmacy/over the counter) – Use as directed on box/bottle.
- Examples: Florastor for Kids
- Culturelle for Kids Flora Q
- Lactinex Granules
Download our PDF print version on Diarrhea in Children. Please contact our office with any questions.
Discipline for Your Child
The Elements of Child Discipline
There are two major reasons for discipline. The first is to protect your child from danger. The second is to teach your child right from wrong and start to teach them reasonable limits and respect for the needs of others.
It is important to establish your rights as a parent first and foremost as you teach your child to respect the rights of others. Infants as young a 4-5 months old can learn to understand no and be taught things such as not to bite Mom with their newly emerged teeth during breastfeeding. While children do not really develop good self-control until age 3-4 years, they need to start being given external controls as early as 6 months to protect them and help them eventually learn self-control.
Rule Setting
- Begin discipline at 6 months of age. Apart from things such as biting while nursing or pulling hair, babies younger than 6 months do not need to be disciplined. As they learn to crawl, however, they need rules for their own safety.
- Be concrete, clear, and brief. Infants and toddlers will not understand nor can they usually attend to a long lecture or series of instructions. They need simple clear rules such as “Don’t push.”
- Be sure to state what the appropriate action is. Make sure your child is aware of what you want her to do. An example
- would be: “I need you to sit here and look at these books until I get off the phone.”
- Ignore trivial misbehavior to avoid constant criticism. This is in the “pick your battles” category. We want to have a healthy relationship with our children, and while we have a lot to teach them, we do not want to come off as totally negative.
- We want to praise them when they do listen and are behaving appropriately. Also, toddlers are natural explorers, and many of the things they want to do are potentially dangerous. Since there are so many things we must prohibit for their own good, we do not want to belabor trivial things such as swinging their legs or occasional whining.
- Give rules that are fair and reasonable for the child’s developmental level.
- Children should not be punished for behavior that is part of a child’s emotional development, such as thumb sucking, toilet training accidents, or separation anxiety. They should be comforted when these things occur and encouraged that things will get easier as they get a little older.
- Prioritize rules and concentrate on just a few initially. Safety rules such as “You must never run out into the street” are the highest priority. After safety, the second priority is respect for property and avoiding any behavior that damages the property (yours and especially belonging to others). After those two major ones, then we tackle issues such as whining or throwing tantrums.
- Apply the rules as consistently as possible. As parents, we are only human, and there will be times we may not follow through or times we should overlook our own rules, but in general, the more consistent we are, the easier it will be for our children to learn to follow the rules.
Techniques for certain ages
- 6 months to 3 years: Structured home environment, distraction, ignoring, verbal and nonverbal disapproval, physically moving or escorting, brief time-out.
- 3-5 years: Techniques above especially time-out, natural consequences, and logical consequences. Restriction places for certain behaviors.
- 5 years – teenage: Techniques above in addition to delay or removal of privilege, negotiation via family meetings
- Adolescence: Logical consequences, “I” messages, family meetings about house rules.
- Structured home environment: Keep your infant and toddler out of harm’s way by putting up gates and cabinet locks. We want to allow the child as much freedom as possible to play and roam without getting into trouble. Movable gates to allow a safe play yard are often a great idea, which allows the child to play and have fun without having to be reprimanded.
- Distraction: Helping your upset child get interested in something else is very useful, especially when in public or at someone else’s house.
- Ignore harmless misbehavior: If your child is in a safe place and not causing disturbance to others (at home), ignoring a temper tantrum is usually the best course of action. Ignoring is also helpful for such behaviors as whining, bickering, or interrupting.
- Verbal and nonverbal disapproval: This can be as simple as getting close to your child, looking him right in the eye, and saying a firm “No.”
- Physically moving or escorting: Manual guidance is when you physically move your child from one place to another, such as to bed, to the bath, time-out chair, etc against his will, helping him as much as needed (carrying him if he will not allow himself to be led).
- Time-out: The concept of time-out, which we typically begin at age 2, is to remove our attention from the child in response to persistent lack of cooperation or misbehavior. The child is removed from the place of misbehavior to a boring place such as a playpen or corner of a room. Avoid using the child’s bedroom or crib for this as to not cause association of sleep with punishment. Sometimes we must physically hold a young child in time-out if they will not stay, but we are careful not to look at, talk to, or play with the child in this scenario.
- Generally, the time spent in time out is one minute for each year of age. Setting a timer is essential for this technique to avoid keeping the child in too long or too short.
- Restriction of location for certain undesirable behaviors: There are some behaviors and habits that children develop that take a long time to extinguish or that may never be fully extinguished but must be taught are not socially acceptable to occur in public. Examples of this are nose picking or scratching or touching one’s private parts. If your child does not immediately cease this behavior when you request it, you can have the child go to his room until he stops. This can help avoid power struggles.
- Natural consequences: Your child can learn from poor choices that are not too dangerous. For example, refusal to wear a coat when going outside to play will cause the child to be uncomfortably cold. Insisting on playing roughly with a particular toy may result in its breakage, and then the child will no longer have that toy.
- Logical consequences: These are consequences parents assign that are logically related to the misbehavior. For example, misusing a possession will result in its removal or loss of a certain privilege for a finite period of time.
- Delay a privilege: This is a logical rule to enforce such as “No television until after homework is done.”
- “I” messages: This is when you tell your child how her behavior makes you feel. An example would be: “I get upset when you leave your room looking like this.”
- Family meetings: As children get older, family meetings are a good tool to discuss rules and problems. You can encourage participation from children by asking questions such as “What are some ways we could solve this problem that you think would be fair?” You may not choose to implement the child’s suggestion, but allowing him a voice in the matter empowers him to start thinking about coming up with solutions, rather than just telling you the problem.
- Avoid physical punishment: Physical discipline is the least likely to be effective and can often inflame the situation with a child who is out of control and prompt the child to possibly hit back. While usually to be avoided, a quick swat to the behind of a child who does something dangerous (such as darting out
- into the street) can be very effective when spanking is otherwise never used.
- Avoid yelling: Yelling causes an angry child to want to yell back and teaches the child to yell when she is angry. While it is difficult to maintain one’s composure all the time, it is a goal to work towards. Your child will be calmer in the long run if you pattern staying calm.
- Catch your child being good: It is extremely important to notice when your child is behaving in the manner you desire. Praise your child for the desired behavior. Studies have shown that praising your child for particular behaviors increases his motivation to continue the behavior. Saying “I am so impressed by how you continued to work out that problem until you came to the right answer. That shows persistence” is much more effective than “You are such a smart boy.”
Hints for effective consequences
- Be clear and brief. Follow through on what you tell your child.
- Be kind. Talk to your child the way you want others to talk to you. You can begin by empathizing with your child, saying something like “I wish I could let you keep coloring, but now it is time to get ready for bed.”
- Apply consequences immediately. If your child no longer remembers why she is being punished, it won’t be very effective.
- Concisely remind your child why he is being punished. State the infraction in one sentence, and then restate the rule. “You are losing your hour of TV time because you hit your sister. We do not hit.”
- Ignore your child’s arguments while you are correcting her. This is a way children delay punishment.
- Discuss the behavior at a later time, but avoid engaging in argument in the moment.
- Keep punishments brief and reasonable. A preferred toy should be taken away for hours or a day, not weeks. Time out is 1 minute per year of age with a maximum of 10 minutes.
- Once the child serves the consequence, embrace him. Do not comment on the previous misbehavior, but start anew.
- Be specific about the infraction and do not generalize to make comments about the child. An example would be to say, “Throwing food is unacceptable. You are in time out for 4 minutes.” We would never want to say, “You are a bad girl.”
Recommended Reading
Adele Faber and Elaine Mazlish, How to Talk So Kids Will Listen and Listen So Kids Will Talk.
Foster Cline and Jim Fay, Parenting with Love and Logic.
Download our PDF print version of Child Discipline. Please contact our office with any questions.
Eczema Care
Eczema Care for Children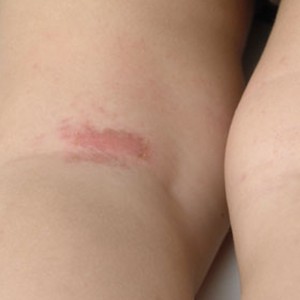
Eczema in children is a skin condition that has no cure that results in dry, itchy, red, and irritated skin. For many people eczema is an inherited condition, for some it is an allergic reaction, and for others there may not be a clear explanation for why they have it. Despite the cause, the management of eczema is similar for all types. Below are instructions for how to best care for your child’s eczema.
Bathing
Increasing the moisture content of the skin is the primary treatment of eczema and frequent bathing is a way to do this. We recommend the following:
- When bathing, avoid soaps and use soapless cleansers like Cetaphil, Aquanil, Aquaphor, or CeraVe instead.
- Give your child daily 10-20 minute soaking baths (until pruning occurs)
- Immediately apply moisturizer to your child after the bath, this is the key to sealing in moisture from the bath. Do not towel dry the child, instead wipe off excess water with your hands and apply the moisturizer to the damp skin.
- Bathing may be more effective if oil is added to the bathwater. Sunflower oil is a good choice as it is anti-inflammatory and inexpensive. If oil is added to the bathwater, do not rinse it off of the child prior to moisturizing.
- If your child has an eczema flare requiring topical steroids, apply the medication to the skin prior to moisturizing. However, if you are not able to apply the steroid in less then 3 minutes after the bath, then wait to apply the steroid until after moisturizing has occurred. In order for moisturizing after the bath to be effective, it must occur within 3 minutes of getting out of the bath.
- For children with recurrent skin infections, adding household chlorine bleach to the bath (1/4 – ½ cup in a tub of water) will reduce the amount of bacteria on the skin and reduce the recurrence of infection as well as help the eczema heal. If you are not sure if your child would benefit from bleach baths, ask your doctor.
Moisturizers
The best moisturizer is the one that works best for your child. In general, ointments are better than creams which are better than lotions. However, ointments leave the skin sticky and shiny and may not be suitable for use during the day. If you or your child can’t tolerate using an ointment during the day, use a cream during the day and use the ointment before bed. The following are moisturizers that we like:
- Aquaphor Ointment
- Aveeno Baby Eczema Cream
- CeraVe Moisturizing Cream
- Cetaphil Restoraderm
- Curel Itch Defense Lotion
- Eucerin Eczema Relief Cream
- Triple Cream
- Vaseline Original Jelly (rated the best by the National Eczema Association)
Topical Steroids
Despite your best efforts, all children with eczema experience flares where their skin gets red, irritated, and itchy. Often it is necessary to use steroid treatments to calm the inflammation and improve the eczema. For most children, a low potency over-the- counter steroid like 1% Hydrocortisone is sufficient to treat the eczema. If a stronger steroid is needed, you will need to consult your doctor. When used appropriately, topical steroids are very safe. Be sure the follow these recommendations for safe, effective use:
- Apply steroids only to the rough affected skin and avoid normal skin unless directed otherwise by your doctor.
- Avoid use on eyelids
- Avoid applying steroids in the diaper area unless directed to by your doctor
- Do not apply steroids more than twice a day
- Do not use steroids for more than 2 weeks in a row unless directed by your doctor
Wet-to-Dry Dressings
It may sound strange, but putting your child to bed in wet pajamas is one of the best treatments for eczema. Despite the popular wives’ tale, putting your child to bed in wet clothes will not give him pneumonia, it will however provide continuous overnight moisturization for his dry skin.
- Leotard style pajamas work best. For the hands use gloves and for the feet use socks.
- Soak a pair of cotton pajamas in warm water then wring out the excess water so that the pajamas are still damp. After bath, moisturization, and topical steroid (if applicable), dress your child in the wet pajamas. Finally, dress them in dry pajamas of the same style so that the wet pajamas are covered by the dry.
- Do the same for socks and gloves if indicated.
Download our PDF print version on Eczema in Children. Please contact our office with any questions.
Flu (Influenza)
What is influenza?
Influenza (“flu” for short) is a highly contagious viral respiratory infection. It affects all age groups but is especially dangerous in small children, infants, and the elderly.
When do you see influenza?
The influenza season usually lasts from late October through March, but outbreaks can arise any part of the year.
What are signs and symptoms of influenza?
- A sudden fever (usually above 101°F or 38.3°C)
- Chills and body shakes
- Headache, body aches, and being a lot more tired than usual
- Sore throat
- Dry, hacking cough
- Stuffy, runny nose
- Some children may throw up (vomit) and have loose stools (diarrhea)
- Infants with the flu also may seem fussy all of a sudden or just “not look right”
How long does influenza last?
Most times, the fever will last upwards of 5 days. The cold symptoms, cough, and fatigue may take up to 1-2 weeks to resolve. It is important to monitor for worsening symptoms because pneumonia and other life-threatening complications can occur.
How contagious is the Flu?
The flu is spread by virus-infected droplets that are coughed or sneezed into the air. People who are infected can spread the virus from a day before they feel sick until their symptoms have ended (about 1 week for adults, but this can be longer for young kids).
The flu usually occurs in small outbreaks, but sometimes can spread quickly. This is known as an epidemic. An epidemic peaks within 2 or 3 weeks after the first cases occur.
When an epidemic spreads throughout the world, it’s known as a pandemic. The most recent flu pandemic occurred in 2009-2010, with the H1N1 (“swine”) flu.
Why should my child get the flu shot every year?
Routine annual influenza vaccination is recommended for everyone 6 months old and older. It’s usually offered between August and mid-November, but may be given at other times of the year.
Each year, researchers try to predict which strains of influenza will spread across the world. The most likely strains are then targeted with upcoming seasonal flu vaccine. While the vaccine doesn’t completely guarantee against getting sick, someone who’s been vaccinated will have fewer and milder symptoms if they contract the virus.
People who got the vaccine one year aren’t protected from getting the flu the next because the protection wears off and flu viruses constantly change. That’s why the vaccine is updated each year to include the most current strains of the virus.
What types of vaccines are available?
There are two types of vaccines available to children. Your health care team will advice you about the best choice of vaccine for your child and family.
- The nasal mist is a live weakened viral vaccine that is sprayed into the nostrils. It is licensed to children 2 years and older. It now is preferred vaccine for children under 9 years old. Some children with severe medical issues are not candidates for this vaccine.
- The injectable vaccine does not contain any live components but still is effective at preventing influenza infection. It is offered to infants as young as 6 months and also is the preferred vaccine for children with certain medical conditions (immunodeficiency, children on chemotherapy, severe asthmatics).
- It can take about 2 weeks after the shot for the body to build up protection to the flu. Getting the shot before the flu season is in full force gives the body a chance to build up immunity to, or protection from, the virus.
What are the side effects of the vaccine?
While very few people get side effects from the seasonal flu vaccine, those who do may have soreness or swelling at the site of the injection or mild side effects, such as a headache or low-grade fever.
Some people who get the nasal spray vaccine also may develop mild flu-like symptoms, including a runny nose, headache, vomiting, muscle aches, and fever. Though these symptoms may appear to be “flu-like”, the vaccine reactions are much less severe than contracting influenza.
It is a common myth that flu vaccine causes the “flu”.
Besides vaccination, what are other ways to prevent acquiring influenza?
- Avoiding large crowds can help during flu season, but it’s often impossible to keep kids cooped up.
- Wash your hands thoroughly and frequently with soap, especially after using the bathroom, after coughing or sneezing, and before eating.
- Never pick up used tissues.
- Never share cups and eating utensils.
- Stay home from work or school when you’re sick with the flu or other serious illness.
- Cover your mouth and nose with a tissue when you cough or sneeze, then put it in the trash. If a tissue isn’t available, cough or sneeze into your upper arm, not into your hands.
What are some home remedies?
- Drink lots of fluids to prevent dehydration.
- Get plenty of sleep and take it easy.
- Take acetaminophen or ibuprofen to relieve fever and aches (do not give aspirin to children or teens as it may cause a rare but serious illness called Reye syndrome).
- Wear layers, since the flu often makes them cold one minute and hot the next (wearing layers — like a T-shirt, sweatshirt, and robe — makes it easy to add or subtract clothes as needed).
What medications are available?
Cases of the flu rarely require specific medical treatment. Some children and especially infants can develop complications (pneumonia, ear and sinus infections) which require antibiotics. Other children may become severely dehydrated and need to hospitalized to receive intravenous hydration.
For a severely ill child or one with other special circumstances, a doctor may prescribe an antiviral medicine that can decrease the duration of illness by 1-2 days and prevent potential complications of the flu. This medicine can only be helpful if it’s given within 2 days of the onset of the flu. Most healthy children who contract the flu do not need to take an antiviral medication.
If any medication is prescribed, be sure to discuss any possible side effects with your doctor.
How long should I keep my child home?
Kids who are sick should stay home from school or childcare until they are without fever for at least 24 hours without relying on the use of a fever-reducing medicine (Tylenol, Motrin, Advil, etc). You may want to keep your child home longer, depending on how he or she is feeling. If you have questions or concerns, talk to your doctor.
When should I call the office?
- Has flu symptoms
- Has a high fever, or fever with a rash
- Has trouble breathing or rapid breathing
- Has bluish skin color
- Is not drinking enough fluids or constantly vomiting
- Is urinating less than 3 times a day
- Seems very sleepy or lethargic
- Seems confused or irritable
- Has symptoms that get better, but then get worse
- Recommended resources
CDC website
Healthychildren.org
Download Influenza PDF
Herpangina & Hand-Foot-And-Mouth
Both viral syndromes are caused by coxsackie viruses. About half of all children with coxsackie virus infection have no symptoms. In addition to fever, coxsackie viruses usually cause one of two primary patterns of illness.
Herpangina
- Usually caused by group A coxsackie viruses.
- Often in the summer or early fall, typically 3-10 years old.
- Small blisters at the back of throat, especially near the tonsils and/or roof of the mouth. Blisters can rupture to form larger ulcers.
- Can also have headaches, vomiting or abdominal pain.
- Oral lesions usually resolve spontaneously in less than 3-5 days.
Hand-Foot-And-Mouth
- Usually caused by A16 coxsackie virus (less commonly enterovirus 71). Often in spring or early summer, most commonly less than 5-10 years old. Small blisters on the tongue, gums, inside of cheeks, and roof of the mouth.
- Small tender blisters on the hands and/or feet (especially palms or soles and between fingers or toes), buttocks and genitals.
- Typical symptom resolution: Fever up to 3 days, mouth ulcers up to 7 days, rash on hands, feet and/or diaper area up to 10 days.
- A 16 coxsackie virus can also cause fingernail or toenail changes over the next few months.
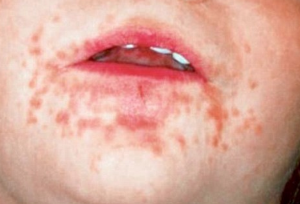
Contagiousness
- Coxsackie viruses are contagious but typically cause mild and harmless disease.
- A child may return to child care or school after the fever is gone, drooling from mouth sores has stopped, and the child’s needs do not compromise the staff’s ability to care for other children. Most children are able to return after the first few days of the illness.
- Coxsackie viruses are passed from person to person on unwashed hands or surfaces contaminated by stool and can also be spread through droplets of fluid sprayed into the air when someone sneezes or coughs.
- The typical incubation period (time from exposure to symptom onset) is 3-6 days. The rash is not contagious.
Care Advice
- Fever and/or pain control as needed for comfort.
- Liquid antacid (such as Maalox) up to 4x/day after eating as needed Encourage cool fluids via cup, spoon, or syringe.
- Soft, non-acidic, non-spicy foods as tolerated.
When to Call
- Child looks or acts very sick.
- Signs of dehydration (very dry mouth, no tears, no urine for more than 8 hours).
- Stiff neck, severe headache, or acting confused. Very red, swollen and tender gums.
- Heavy breathing and/or excessive tiredness even when there is no fever. Fever above 101F for more than 3 days.
Prevention
- Hand washing is the best mode of prevention (www.cdc.gov/handwashing).
- Emphasize hand washing after using the toilet, after changing diapers, before preparing food meals, and before eating meals.
- While your child has a fever, avoid swimming pools or sharing a bath with another child.
Download our PDF print version on Herpangina & Hand-Foot-And-Mouth in Children. Please contact our office with any questions.
Hives (Urticaria)
What are Hives (Urticaria)?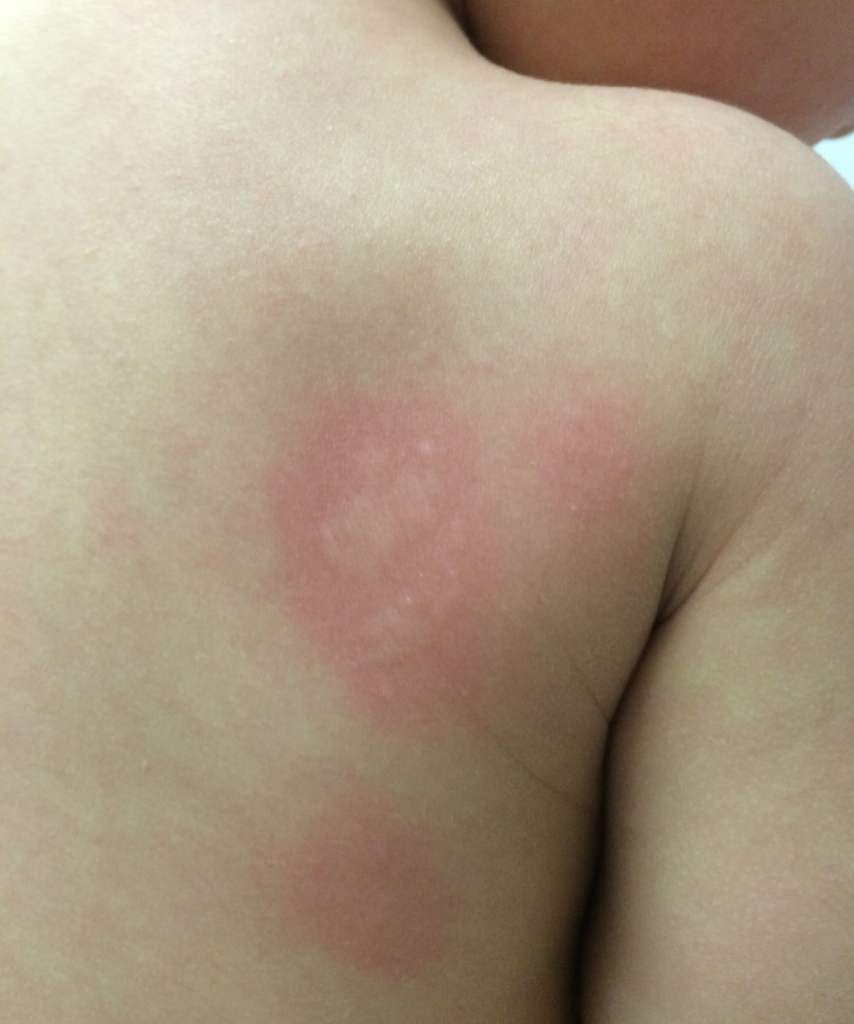
Hives (Urticaria) are itchy, raised pink or red bumps with pale centers. These spots often resemble mosquito bites and can be different shapes and sizes. Hives can occur all over the body, or they may be localized to one area. The location and appearance of the rash frequently changes, often within a matter of hours. Hives do not spread from person to person. Most commonly, they come and go for a few days before spontaneously resolving. More than two-thirds of all cases completely go away within six weeks.
What causes hives?
Most cases of hives in children result from a response to an infection, most commonly a virus. An allergic reaction to a medication, food, plant, detergent or other substance can also cause this type of rash. Foods that are most often associated with hives include peanuts, tree nuts, egg whites, shellfish, milk, and sesame. Bee stings and insect bites can also result in hives. It is important to note that, in many cases, the exact cause of the rash cannot be determined. If your child’s doctor suspects a serious allergy, then further testing and/or referral to a specialist may be indicated.
How do I care for my child?
Treatment for hives often consists of supportive care.
- Give your child an antihistamine medication. This medicine won’t cure the hives, but it will help the itching and reduce the number of hives. Use the specific medication recommended by your child’s doctor. Continue the medicine until you are sure the hives are completely gone for 24 hours. Otherwise, your child may get itchy again.
- Apply cool compresses to the area of itching and swelling to help relieve symptoms.
- Avoid heat and washing with hot water. This can make hives worse.
- Make sure your child stays away from anything you think may have caused the hives.
Additional interventions may be necessary if it appears that internal parts of the body are involved in the allergic reaction. If your child is wheezing or having trouble breathing or swallowing, you should seek emergency treatment.
When should I seek medical treatment?
Call 911 or go to the Emergency Room if your child has the following:
- Wheezing or difficulty breathing
- Rapid onset cough or hoarseness
- Difficulty swallowing or speaking
- History of severe life-threatening allergic reaction to a similar substance Call your child’s doctor immediately if your child has the following:
- Severe hives (eye/lip swelling, very itchy, etc)
- Abdominal pain, vomiting, or diarrhea
- Acting very sick
Call your child’s doctor during office hours if
- The rash has not significantly improved after taking an antihistamine for 24 hours.
- You have additional questions or concerns.
Download our PDF print version on Hives in Children. Please contact our office with any questions.
Probiotics
Probiotics (PDF)
Probiotics are beneficial microorganisms that are naturally found in the intestines. The human digestive tract normally contains hundreds of types of bacteria that reduce the growth of harmful bacteria and promote a healthy immune system. Illnesses and treatment with antibiotics can alter this healthy balance. There are a wide variety of foods and over-the-counter supplements that can help restore the beneficial flora in the gut. Probiotic supplements can be found at most pharmacies and natural or health-food stores, although you may need to ask the pharmacist. Some products need to be refrigerated. Specific brands that can help with different medical issues are listed below.
Colic
Gerber Soothe Colic Drops (formerly known as BioGaia)
Antibiotic-associated diarrhea
Florastor/Florastor Kids
Common Diarrhea/Intestinal Health
Culturelle/Culturelle Kids
VSL#3
FloraQ
Jarrow Yum-Yum Dophilus
Lactinex Granules
Female Urinary Tract Health/ UTI prevention
Jarrow Fem-Dophilus
Skin rashes in Children
Tips for Picky Eaters
 It is very normal for children of all ages to have a few food dislikes. About 20% of toddlers and young children are picky eaters and have several food dislikes. Children who are picky eaters may choose 1 or 2 preferred foods and refuse to eat other foods for weeks at a time. They may also be unpredictable about their food preferences, with their predilection for a particular food varying on a day-to-day basis. It is common for young children to dislike foods with a bitter or spicy taste. Often, children will reject a food because it is difficult to chew. Try not to worry too much about this behavior, since most children outgrow it by the early school years.
It is very normal for children of all ages to have a few food dislikes. About 20% of toddlers and young children are picky eaters and have several food dislikes. Children who are picky eaters may choose 1 or 2 preferred foods and refuse to eat other foods for weeks at a time. They may also be unpredictable about their food preferences, with their predilection for a particular food varying on a day-to-day basis. It is common for young children to dislike foods with a bitter or spicy taste. Often, children will reject a food because it is difficult to chew. Try not to worry too much about this behavior, since most children outgrow it by the early school years.
Tips for Picky Eaters
- Trust your child’s appetite to balance out his caloric needs.
- Avoid praising your child for eating. Don’t give bribes or rewards for meeting your eating expectations. Children should eat to satisfy their appetite, not to please the parent.
- Keep the mealtime atmosphere pleasant. Try to make it an important family event. Draw your children into friendly conversation. Talk about fun subjects unrelated to food. Avoid turning it into a time for criticism or struggle over control
- Try to serve a main dish that everyone in the family likes. Some children don’t like foods that are mixed together, such as casseroles. Try reintroducing such dishes when your child is older.
- Allow occasional substitutes for the main dish, but avoid getting into the habit of being a “short-order cook.” Have a few nutritious, easy-to-prepare items on hand (cereal, simple sandwiches, yogurt) as substitutes for the main entrée. Your child should understand that you eventually want him to eat the main dish that has been prepared for the whole family.
- Respect any strong food dislikes. If your child has a few strong food dislikes (especially any food that makes him gag), do not serve that food to him even when it is prepared as part of the family meal.
- Don’t become overly-concerned or make your child feel guilty for refusing vegetables. This is very common, and a well-balanced diet is still possible. Continue to encourage nutritious foods in general. Try serving vegetables that are well-cooked and easy to chew. Consider getting creative and using fun names (broccoli trees, carrot spears, etc) to encourage vegetable consumption. Serving dips and spreads may also help. You can even “sneak” vegetables into certain dishes or incorporate them into smoothies.
- Discourage complaining about food at mealtimes. Initiate a rule that it’s okay to decline a serving of a particular food or to push it to the side of the plate, but complaining or whining about it is unacceptable.
- Encourage your child to taste new foods. Many tastes are acquired, and your child may eventually learn that he likes a food that he initially refused. Research indicates that it may take seeing other people eat a new food 10 times before a child is even willing to taste it, Then, it may take another 10 times of tasting it before they develop a liking for it. Don’t try to rush this normal process of adapting to new foods.
- Avoid pressure or punishment at mealtime. Don’t pressure, beg, or bribe your child to eat all foods. Don’t punish your child for refusing to take one bite of a new food. It will only lead to liking that food less over time. If your child has a stubborn, strong-willed nature, pressure around eating can progress to a power struggle, which in turn prolongs the picky eating.
- Don’t argue about dessert. An unnecessary area of friction for picky eaters is a rule that, if you don’t clean your plate, you can’t have any dessert. A better approach is to allow your child one small portion of desert no matter what he eats. And remember–desserts don’t always have to be sweets; they can be more nutritious foods like fruits or yogurt.
- Don’t argue about a bedtime snack. If your child complains about bedtime hunger, avoid a long discussion. Give him a small, plain snack (such as cereal) before it is time to brush his teeth.
- Don’t extend mealtime. Don’t keep your child sitting at the dinner table after the rest of the family is done. This will only cause your child to develop unpleasant associations with mealtime. If he suddenly wants to eat, give him 5 extra minutes to do so.
Download our PDF print version on Tips for Picky Eaters. Please contact our office with any questions.
Toilet Training your Child
 Few things are as anxiety-provoking for parents as toilet training. As if coercing your child to use the potty and dealing with inevitable accidents are not enough, parents also have to deal with comparisons to other children and the feeling that the ability to potty train is not only a judgment on the child’s development and intelligence but also a judgment on the parent’s ability to parent.
Few things are as anxiety-provoking for parents as toilet training. As if coercing your child to use the potty and dealing with inevitable accidents are not enough, parents also have to deal with comparisons to other children and the feeling that the ability to potty train is not only a judgment on the child’s development and intelligence but also a judgment on the parent’s ability to parent.
We have all met, or at least heard of, the parent who proudly shares that her child was potty trained at 24, 18, 12, or even 6 months of age. If you are that parent, congratulations, getting your child toilet trained is something to be proud of no matter what the age. But if you are the parent who feels a slight twinge of failure when confronted with the toilet training accomplishments of your friends, this article is for you.
If you take nothing else from this article, I want you to take home the message that children toilet train on their own time, the age at which a child becomes toilet trained has no relationship to his intelligence, and the age at which a child becomes toilet trained says nothing about how “good” a parent is.
If toilet training happens when the child is ready, when is that? Before children are 12 months of age, they do not have control over their bladder or bowel movements. Some parents are able to recognize the signs that their child is about to urinate or have a bowel movement, and as a result, are able to achieve a form of pseudo-toilet training at a young age. True toilet training, however, cannot occur until a child is able to control her bowels and bladder, which often occurs between 18 and 24 months. However, some may not achieve this control until 30 months or older, which is normal. Even if your child is able to stay dry during the day, it is important to remember that it may take months or years for your child to be dry at night. For most children, the ability to stay dry at night does not come until after they are 5 years old.
Regardless of your child’s age, the following are signs that your child may be ready for potty training:
- Your child stays dry at least two hours at a time during the day or is dry after naps.
- Bowel movements become regular and predictable.
- You can tell when your child is about to urinate or have a bowel movement.
- Your child can follow simple instructions.
- Your child can walk to and from the bathroom and help undress.
- Your child knows the difference between wet and dry.
- Your child asks to use the toilet or potty chair.
- Your child asks to wear “big–kid” underwear.
If you have determined that your child is ready to begin the toilet training process, the following tips from the American Academy of Pediatrics can help you achieve success.
1. Decide what words to use to describe body parts, urine, and bowel movements. It is best to use proper terms that will not offend, confuse, or embarrass anyone.
2. Pick a potty chair. They are logistically easier for a small child to use because there is no problem getting onto it, and a child’s feet can reach the floor. If you use a child-size seat attached to an adult toilet, make sure you provide a step stool to support the feet so she can push down during bowel movements.
3. Be a role model. Children are often interested in their family’s bathroom activities. It is sometimes helpful to let children watch the parents when they go to the bathroom. Seeing grown-ups use the toilet (and wash their hands afterward) makes children want to do the same. If possible, mothers should show the correct skills to their daughters, and fathers to their sons. Children can also learn these skills from older brothers and sisters.
4. Know the signs. Before having a bowel movement, your child may grunt or make other straining noises, squat, or stop playing for a moment. When pushing, his face may turn red. Explain to your child that these signs mean that a bowel movement is about to come. Your child may wait until after the fact to tell you about a wet diaper or a bowel movement. This is actually a good sign that your child is starting to recognize these body functions. Praise your child for telling you, and suggest that “next time” he let you know in advance. Keep in mind that it often takes longer for a child to recognize the need to urinate than the need to move bowels.
5. Make trips to the potty routine. When your child seems ready to urinate or have a bowel movement, go to the potty. It may also be helpful to make trips to the potty a regular part of your child’s daily routine, such as first thing in the morning, after meals, or before naps. Keep your child seated on the potty for only a few minutes at a time and explain what you want to happen. (It is better for boys to learn to urinate sitting down first.) In the beginning, many children have bowel movements or urinate right after getting off the toilet. It takes time for children to learn how to relax the muscles that control the bowel and bladder. If this happens a lot, it may mean your child is not ready for training.
6. Teach your child proper hygiene habits. Show your child how to wipe carefully. (Girls should wipe thoroughly from front to back to prevent bringing germs from the rectum to the vagina or bladder.) Make sure both boys and girls learn to wash their hands well after urinating or after a bowel movement.
7. Praise your child. Encourage your child with lots of hugs and praise when success occurs. When a mistake happens, treat it lightly. Punishment and scolding will often make children feel bad and may make toilet training take longer.
8. Incentivize staying dry. If you are going to use incentives to encourage potty training, give them for staying clean and dry, and not for using the potty. Giving rewards for using the potty creates a situation where the child is in control because only she can decide if she pees or poops. If your child should decide she does not care about going to the potty, the incentive becomes useless. By incentivizing staying clean and dry, the parent is in control of the training process and is able to continually remind the child of the importance of staying dry.
9. Try training pants. Once your child starts using the potty with some success, training pants can be used. This moment will be special. Your child will feel proud of this sign of growing up. However, be prepared for “accidents.” It may take weeks, even months, before toilet training is completed. Continue to have your child sit on the potty several times during the day. If your child uses the potty successfully, it is an opportunity for praise. If not, it is still good practice. Some children who are not ready for training pants will still feel that they are more “grown up” if they wear disposable training pants (Pull-ups is one brand name) as a step forward in the training process. Some children will want to go back to diapers, especially for bowel movements. Instead of looking at this as a failure, praise your child for knowing when he needs to go. Suggest that he have the bowel movement in the bathroom while wearing a diaper. Encourage improvements, and work toward sitting on the potty without the diaper.
10. Avoid a power struggle. Children at toilet training ages are striving for independence and are becoming aware of their individuality. They often look for ways to test their limits, and some may do this by holding back bowel movements. Do your best to stay relaxed about toilet training. Remember that no one can control when and where a child urinates or has a bowel movement except the child.
11. Understand their fear. Some children believe that their wastes are part of their bodies, and seeing their stools flushed away may be scary and hard to understand. Some also fear they will be sucked into the toilet if it is flushed while they are sitting on it. To give your child a feeling of control, let her flush the toilet. For those children who are still having bowel movements in their diaper, it may be helpful to empty the contents of the diaper into the toilet and flush it as the child observes. This will lessen the fear of the sound of rushing water and the sight of things disappearing while reinforcing that bowel movements belong in the toilet.
Hopefully, these tips give you the tools you need to approach toilet training successfully and with minimal stress. These tips are helpful for all children and provide an easy introduction to the toilet training experience. There are other more aggressive strategies for toilet training children that take only “three days,” however; these strategies are intended for the child who has already demonstrated some potty training success or ability to control bowel and bladder function.
Should you feel like your child is struggling with toilet training, talk with your pediatrician. Most of the time the problem is minor and can be resolved quickly,
but sometimes physical or emotional impairments will require treatment. The most common physical impediment to successful toilet training is constipation. If your child has frequent accidents, pay close attention to the character and consistency of her bowel movements. If her stools are consistently hard, large, or look like pebbles or rocks, then constipation is likely, and she would benefit from treatment by your pediatrician. You should also keep in mind that major changes in the home, like moving or the birth of a sibling, may result in toilet training regression. Should you notice a change in the home environment affecting your child’s toilet training, take the time to address his emotional needs before trying to advance.
If you find that all of the tips and strategies that friends, family, and your pediatrician provide are not helping, consider reading the book Stress-Free Potty Training: A Commonsense Guide to Finding the Right Approach for Your Child by Sara Au and Peter L. Stavinoha. This book is unique in that it does not provide a singular approach to toilet training. Instead, it provides five different approaches specific to different personality types. For the child who is resistant to conventional toilet training strategies, this book can be very helpful.
Good luck!
Download our PDF print version on Toilet Training. Please contact our office with any questions.
Uncircumcised Penis Care
Basics
If your son is uncircumcised, then he will have a layer of skin (foreskin) covering the head if the penis. Usually, the foreskin remains tightly adherent to the tip of the penis for the first few years of life. In most boys, the foreskin separates, or retracts, from the tip on its own by age 5.
Sometimes, the foreskin may not retract fully until puberty. This is still normal—just check with your child’s doctor if you have concerns. You should NEVER forcefully pull the foreskin back to clean the penis. Doing so can lead to complications, including significant pain, bleeding, and tears in the skin.
Cleaning Tips
- Prior to separation of the foreskin (typically before 5 years of age), simply wash the area gently with mild soap and water during bath-time. Do not try to force the foreskin back to clean underneath.
- Once the foreskin has separated, gently pull the foreskin away from the tip of the penis and wash underneath with mild soap and water. Always push the foreskin back over the head of the penis afterward. Cleaning the foreskin should be part of the daily routine.
- Note that, as the foreskin separates, dead skin cells, called smegma, can accumulate. These may look like white lumps underneath the foreskin. Smegma is normal and will go away on its own.
Complications
- Phimosis occurs when the foreskin remains tight and difficult to pull back after puberty.
- Paraphimosis occurs if the foreskin is pulled back and gets “stuck” (cannot be manually pushed back over the head of the penis).
- Always seek medical attention if the penis appears red or swollen, or if an abnormal urinary stream is noted.
Download our PDF print version on Uncircumcised Penis Care. Please contact our office with any questions.
Warts
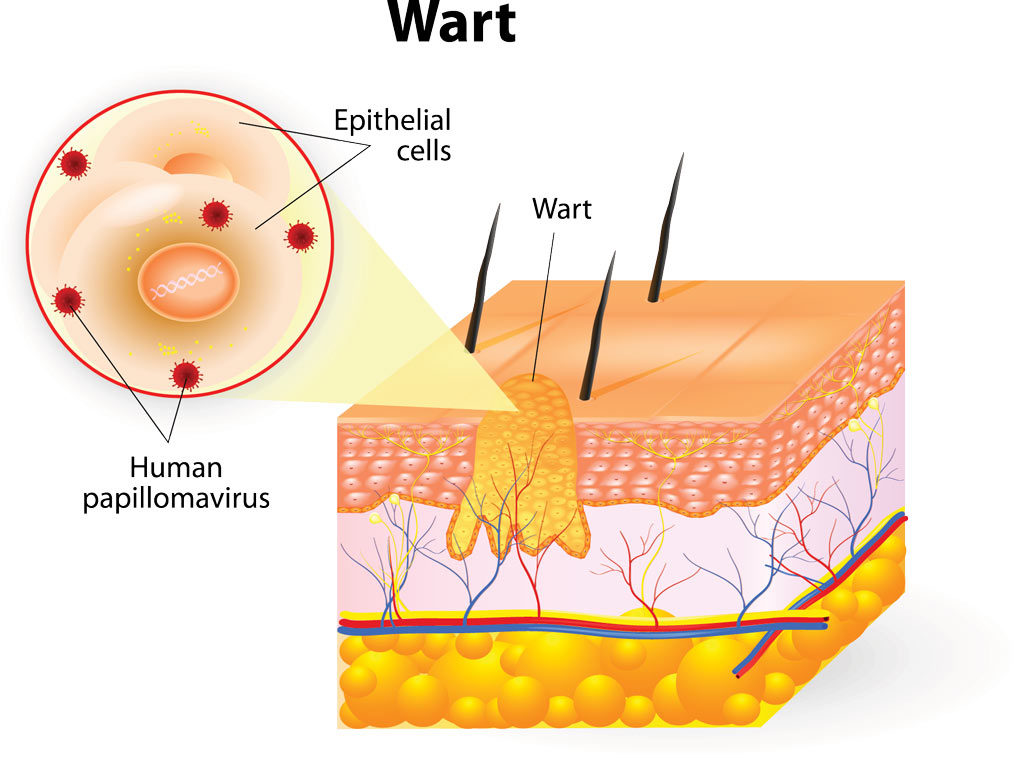 Warts are actually a viral infection that involves the skin top layers. The infection is caused by a family of viruses called human papillomavirus or HPV for short. These infections are more common in children than adults. They can attack any area of the body but the infection starts in a warm, moist environment or areas that have been traumatized. The infection is slow and starts as one lesion but can progress to multiple lesions.
Warts are actually a viral infection that involves the skin top layers. The infection is caused by a family of viruses called human papillomavirus or HPV for short. These infections are more common in children than adults. They can attack any area of the body but the infection starts in a warm, moist environment or areas that have been traumatized. The infection is slow and starts as one lesion but can progress to multiple lesions.
Kids can get warts anywhere (i.e., from touching anything someone with a wart has used, like towels and surfaces, biting or picking their finger and toe nails).
Types of warts
- Common warts Found mostly on fingers, hands, knees, and elbows. A common wart is a small, hard dome-shaped bump. The color be light gray to brown. It has a rough surface similar to a head of cauliflower.
- Flat warts Small (size of a pinhead), flat, and smooth lesions. The color may be pink, light brown, or yellow. The lesion can appear all over the body but most commonly seen on face and exposed extremities
- Plantar warts These warts are common warts found on the sole of the feet and can be very painful. They feel like a piece of glass is caught in the foot.
- Filiform warts Finger shaped, flesh-colored, and grows mostly on or around the mouth, eyes, or nose.
Are Warts Contagious?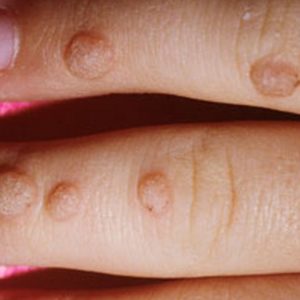
Warts are contagious but not easily transmitted. The wart virus is passed from person to person by close physical contact or from a surface such as a bathroom floor or mat. A tiny cut or scratch on the skin can make the skin more vulnerable to contracting warts. Warts grow slowly taking weeks to see them. Picking at a wart can spread warts to other parts of the body.
How can we prevent warts?
There is no way to prevent from being exposed to a wart virus. They are common and only good hygiene including hand washing and keeping open cuts or scratches clean can prevent the spread of the virus.
Waterproof sandals or flip-flops are a good idea in public showers, locker rooms, and around public pools to protect against plantar warts.
What treatments are there?
Warts are a nuisance more than a problem, so it’s not always necessary to have them removed. Without treatment, it can take anywhere from 6 months to 2 years for a wart to go away. A doctor might decide to remove a wart if it’s painful, spreading, or interferes with activities.
Treatment options
- Observation
- Salicylic acid cream and solutions (Duofilm, Dr. Scholl’s Compound W) These are available over the counter. The treatment involves applying the cream or solution to the area daily and covering with a bandage. The next day, the parent will clean the area and remove any white “dead” skin with either a nail file or pumice stone. Repeat until the wart is removed. IT may take several weeks. Salicylic treatment for warts (PDF)
- Freezing Canister (Compound W Freeze Off and Dr. Scholl’s Freeze Away): This product is available for home use but is not as effective as in-office cryotherapy which we offer. Follow the instruction on the canister and remove dead skin in a few days after treatment. You may need to repeat the treatment several times to achieve a cure.
- Duct tape This approach apply an occlusive tape such as duct tape to the lesion for 24-hour intervals. Warts will soften and the dead skin can be removed with file or pumice stone. This is definitely the most economical method but not very effective. Duct tape for warts (PDF)
- Cryotherapy in our office We offer this in-office treatment for warts. The technique is similar the freezing canister treatments but we are able to achieve colder temperature and much more effective result. Depending on the wart size and location, the treatment will take about 20-40 sec. Warts on the sole of the foot may require two to three treatment cycles. There is some discomfort involved with treatment but generally for a brief period. Your child may complain of soreness over the next 1-2 days. The doctors may recommend other OTC treatments to improve results after the area has healed (3-4 days). Some warts (plantar and larger warts) may require repeat visit in 2-week intervals or referral to a dermatologist for further treatments. Cryotherapy aftercare (PDF)
- Surgical removal or laser treatments Rarely is needed but we will refer to dermatologist or podiatrist to address “stubborn warts”




















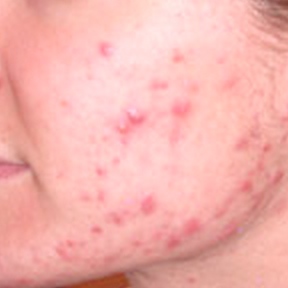

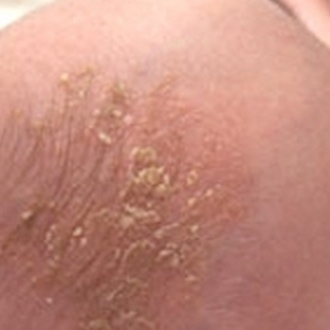
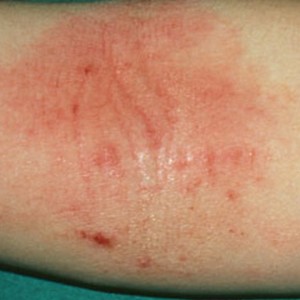
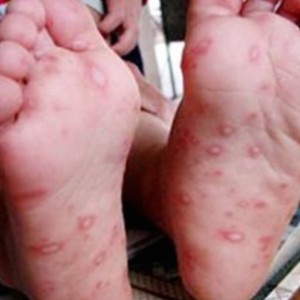

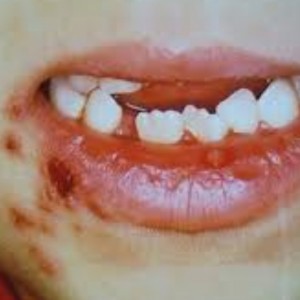
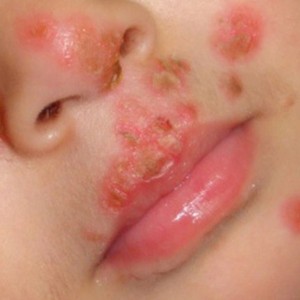
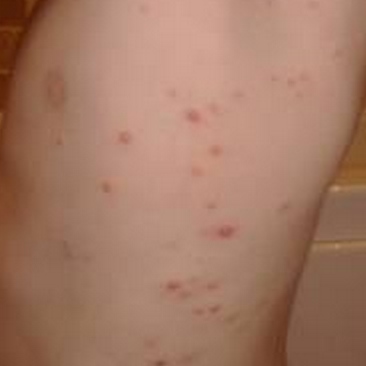
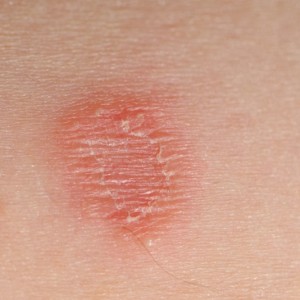
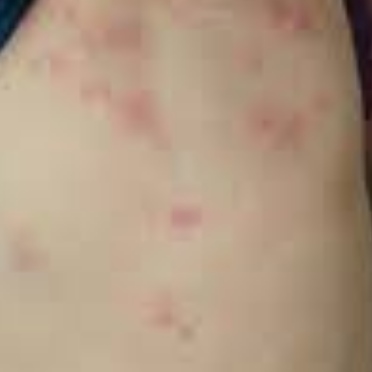
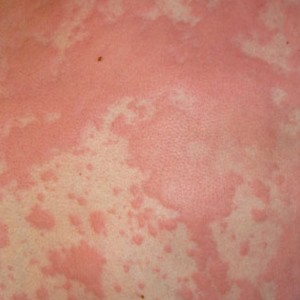
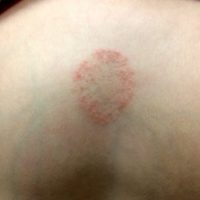
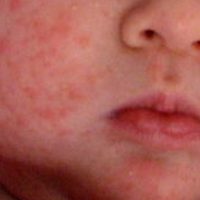

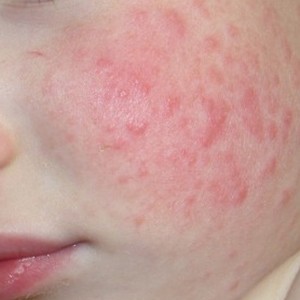
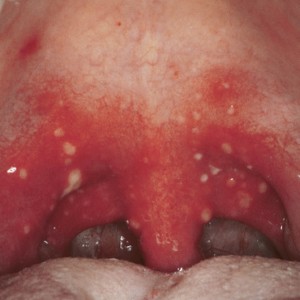
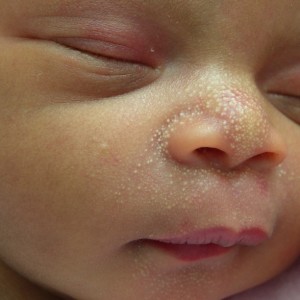
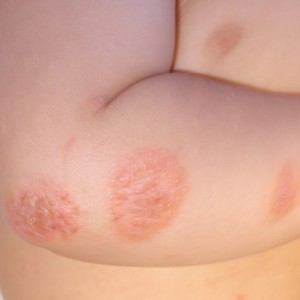
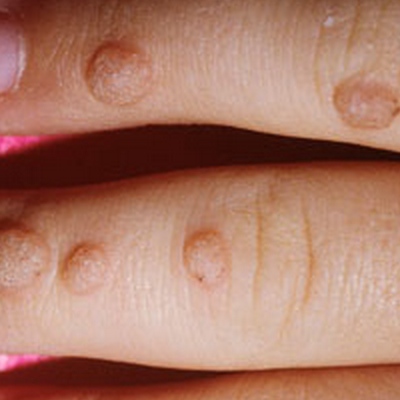

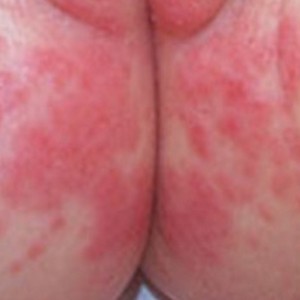
 It is very normal for children of all ages to have a few food dislikes. About 20% of toddlers and young children are picky eaters and have several food dislikes. Children who are picky eaters may choose 1 or 2 preferred foods and refuse to eat other foods for weeks at a time. They may also be unpredictable about their food preferences, with their predilection for a particular food varying on a day-to-day basis. It is common for young children to dislike foods with a bitter or spicy taste. Often, children will reject a food because it is difficult to chew. Try not to worry too much about this behavior, since most children outgrow it by the early school years.
It is very normal for children of all ages to have a few food dislikes. About 20% of toddlers and young children are picky eaters and have several food dislikes. Children who are picky eaters may choose 1 or 2 preferred foods and refuse to eat other foods for weeks at a time. They may also be unpredictable about their food preferences, with their predilection for a particular food varying on a day-to-day basis. It is common for young children to dislike foods with a bitter or spicy taste. Often, children will reject a food because it is difficult to chew. Try not to worry too much about this behavior, since most children outgrow it by the early school years. Few things are as anxiety-provoking for parents as toilet training. As if coercing your child to use the potty and dealing with inevitable accidents are not enough, parents also have to deal with comparisons to other children and the feeling that the ability to potty train is not only a judgment on the child’s development and intelligence but also a judgment on the parent’s ability to parent.
Few things are as anxiety-provoking for parents as toilet training. As if coercing your child to use the potty and dealing with inevitable accidents are not enough, parents also have to deal with comparisons to other children and the feeling that the ability to potty train is not only a judgment on the child’s development and intelligence but also a judgment on the parent’s ability to parent. Warts are actually a viral infection that involves the skin top layers. The infection is caused by a family of viruses called human papillomavirus or HPV for short. These infections are more common in children than adults. They can attack any area of the body but the infection starts in a warm, moist environment or areas that have been traumatized. The infection is slow and starts as one lesion but can progress to multiple lesions.
Warts are actually a viral infection that involves the skin top layers. The infection is caused by a family of viruses called human papillomavirus or HPV for short. These infections are more common in children than adults. They can attack any area of the body but the infection starts in a warm, moist environment or areas that have been traumatized. The infection is slow and starts as one lesion but can progress to multiple lesions.
